Hypereosinophilic Syndrome
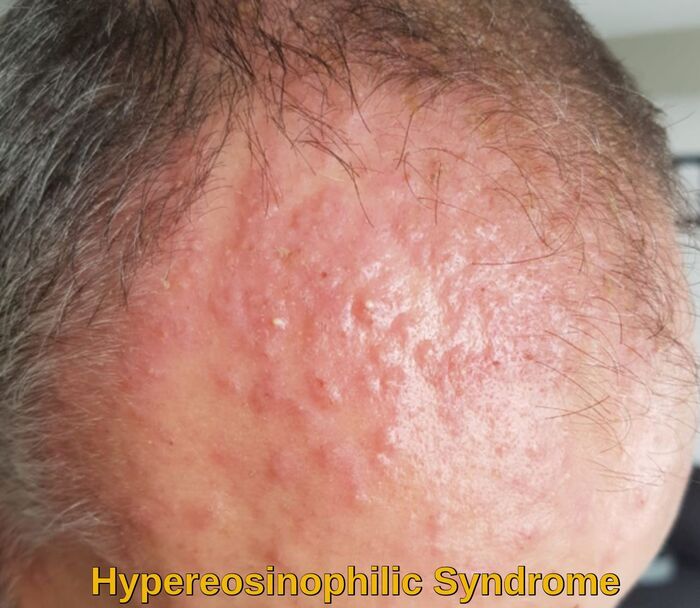
Cutaneous involvement in hypereosinophilic syndrome presenting as erythematous papular and plaque-like lesions on the forehead, reflecting eosinophil-mediated skin inflammation
Hypereosinophilic syndrome (HES) is a rare hematologic disorder characterised by persistent eosinophilia in the peripheral blood, typically with an absolute eosinophil count greater than 1.5 × 10⁹/L, leading to organ damage or dysfunction caused by eosinophil-mediated inflammation and tissue infiltration. Unlike secondary eosinophilia due to parasitic infection, allergy, drug reaction, or autoimmune disease, HES is idiopathic or clonal in nature and requires detailed diagnostic evaluation to identify underlying molecular or myeloproliferative causes. The ICD-10 code for hypereosinophilic syndrome is D72.119. Early recognition, accurate classification, and timely treatment are essential to prevent irreversible complications involving the heart, lungs, skin, and nervous system.
Secondary eosinophilia is a cytokine-derived (interleukin-5 [IL-5]) reactive phenomenon. Worldwide, parasitic diseases are the most common cause, whereas, in developed countries, allergic diseases are the most common cause.
Other causes of eosinophilia include the following:
- Malignancies – Metastatic cancer, T-cell lymphoma, colon cancer
- Pulmonary eosinophilia – Loffler syndrome, Churg-Strauss syndrome, allergic bronchopulmonary aspergillosis
- Connective tissue disorders – Scleroderma, polyarteritis nodosa
- Skin diseases – Dermatitis herpetiformis
- Inflammatory bowel disease
- Sarcoidosis
- Addison disease
- Drug-induced eosinophilia

Common drug classes associated with eosinophilia, including antibiotics, antimalarials, anticonvulsants, NSAIDs, ACE inhibitors, proton pump inhibitors, and other medications implicated in drug-induced eosinophilia
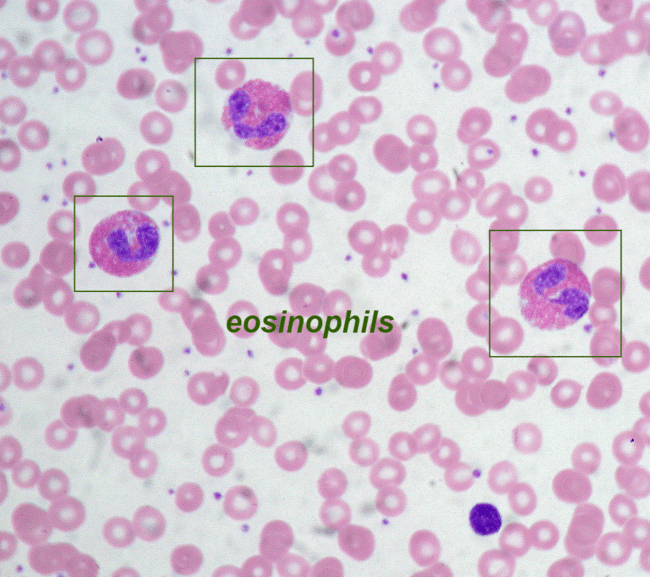
Peripheral blood smear demonstrating eosinophils with characteristic bilobed nuclei and abundant eosinophilic granules, highlighted in the context of eosinophilia and hypereosinophilic syndrome
Hypereosinophilic syndrome is a myeloproliferative disorder characterized by persistent eosinophilia that is associated with damage to multiple organs.
Hypereosinophilic syndrome is traditionally defined as peripheral blood eosinophilia > 1500/mcL (> 1.5 × 109/L) persisting ≥ 6 months.
In 1975, Chusid et al defined the three features required for a diagnosis of hypereosinophilic syndrome:
- A sustained absolute eosinophil count (AEC) greater than >1500/µl, which persists for longer than 6 months
- No identifiable etiology for eosinophilia
- Signs and symptoms of organ involvement
Hypereosinophilic syndrome (HES) was previously considered to be idiopathic but is now known to result from various disorders, some of which have known causes. One limitation of the traditional definition is that it does not include those patients with some of the same abnormalities (eg, chromosomal defects) that are known causes of HES but who do not fulfill the traditional HES definition for degree or duration of eosinophilia. Another limitation is that some patients with eosinophilia and organ damage that characterize hypereosinophilic syndrome require treatment earlier than the 6 months necessary to confirm the traditional diagnostic criteria. Eosinophilia of any etiology can cause the same types of tissue damage.
Hypereosinophilic syndrome is rare, has an unknown prevalence, and most often affects people aged 20 through 50. Only some patients with prolonged eosinophilia develop organ dysfunction that characterizes hypereosinophilic syndrome. Although any organ may be involved, the heart, lungs, spleen, skin, and nervous system are typically affected. Cardiac involvement can cause significant morbidity and mortality.
Symptoms of hypereosinophilic syndrome (HES):
The signs and symptoms of HES can vary significantly depending on which part(s) of the body are affected. Frequent symptoms listed by body system include:
- Skin – rashes, itching, and edema.
- Lung – asthma, cough, difficulty breathing, recurrent upper respiratory infections, and pleural effusion.
- Gastrointestinal – abdominal pain, vomiting, and diarrhea.
- Musculoskeletal – arthritis, muscle inflammation, muscle aches, and joint pain.
- Nervous system – vertigo, paresthesia, speech impairment, and visual disturbances.
- Heart – congestive heart failure, cardiomyopathy, pericardial effusion, and myocarditis.
- Blood – deep venous thrombosis, and anemia.
Affected people can also experience a variety of non-specific symptoms such as fever, weight loss, night sweats, and fatigue.
Occasionally, patients with very severe eosinophilia (eg, eosinophil counts of > 100,000/mcL [> 100 × 109/L]) develop complications of hyperleukocytosis, such as manifestations of brain or lung hypoxia (eg, encephalopathy, dyspnea, respiratory failure). Other thrombotic manifestations (eg, cardiac mural thrombi) may also occur.

Cutaneous manifestations of hypereosinophilic syndrome involving the trunk, presenting as erythematous papules and plaques due to eosinophil-mediated dermal inflammation

Echocardiographic images demonstrating cardiac involvement in hypereosinophilic syndrome with myocardial thickening of the left ventricle (A, arrows), showing marked resolution following corticosteroid therapy (B, arrows)
Subtypes of hypereosinophilic syndrome (HES):
There are two broad subtypes of HES:
- Myeloproliferative variant
- Lymphoproliferative variant
The myeloproliferative variant is often associated with a small interstitial deletion in chromosome 4 at the CHIC2 site that causes the FIP1L1/PDGFRA-associated fusion gene (which has tyrosine kinase activity that can transform hematopoietic cells). Patients often have:
- Splenomegaly
- Thrombocytopenia
- Anemia
- Elevated serum vitamin B12 levels
- Hypogranular or vacuolated eosinophils
- Myelofibrosis
Patients with the myeloproliferative subtype often develop endomyocardial fibrosis and may rarely develop acute myeloid leukemia or acute lymphoblastic leukemia. Patients with the FIP1L1/PDGFRA-associated fusion gene are more often males and may be responsive to low-dose imatinib (a tyrosine kinase inhibitor).
A small proportion of patients with the myeloproliferative variant of the hypereosinophilic syndrome have cytogenetic changes involving platelet-derived growth factor receptor beta (PDGFRB) and may also be responsive to tyrosine kinase inhibitors such as imatinib. Other cytogenetic abnormalities include rearrangement of the gene for fibroblast growth factor receptor 1 (FGFR1) or janus kinase 2 (PCM1-JAK2).
The lymphoproliferative variant is associated with a clonal population of T cells with an aberrant phenotype. Polymerase chain reaction (PCR) shows a clonal T-cell receptor rearrangement. Patients more often have:
- Angioedema, skin abnormalities, or both
- Hypergammaglobulinemia (especially high IgE)
- Circulating immune complexes (sometimes with serum sickness)
Patients with the lymphoproliferative variant also more often respond favorably to corticosteroids and occasionally develop T-cell lymphoma.
Other HES variants include chronic eosinophilic leukemia, Gleich syndrome (cyclical eosinophilia and angioedema), familial hypereosinophilic syndrome mapped to 5q 31-33, and other organ-specific syndromes. In organ-specific eosinophilic syndromes, eosinophilic infiltration is confined to a single organ (eg, eosinophilic gastrointestinal disease, chronic eosinophilic pneumonia).
Hyperleukocytosis may occur in patients with eosinophilic leukemia and very high eosinophil counts (eg, > 100,000 cells/mcL [> 100 × 109/L]). Eosinophils can form aggregates that occlude small blood vessels, causing tissue ischemia and microinfarctions. Common manifestations include brain or lung hypoxia (eg, encephalopathy, dyspnea, or respiratory failure).

Comparison table outlining the main subtypes of hypereosinophilic syndrome, highlighting genetic features, clinical manifestations, associated risks of hematologic malignancy, and treatment responsiveness in myeloproliferative versus lymphoproliferative variants
Diagnosis of hypereosinophilic syndrome (HES):
Symptoms of HES are also common in many other medical problems, making an initial diagnosis more difficult. The first step is to rule out other conditions with similar symptoms. These include parasitic infection, allergic disease, cancers, autoimmune diseases, and drug reactions.
An allergist/immunologist has specialized training to effectively diagnose the problem and, if HES is present, to work collaboratively with other specialists such as a hematologist or cardiologist in the treatment and monitoring of HES.
Testing is individualized according to symptoms and may include stool evaluation to detect parasitic infection, allergy testing to diagnose environmental or food allergies, biopsies of the skin or other organs, blood tests to screen for autoimmunity, CT imaging of affected organs, molecular genetic studies to detect FIP1L1-PDGFRA or other mutations to help determine, diagnosis, prognosis, and treatment. Bone marrow aspirate and biopsy with flow cytometry, cytogenetic testing, and reverse transcriptase-polymerase chain reaction (PCR) or fluorescence in situ hybridization (FISH) is done to identify the FIP1L1/PDGFRA-associated fusion gene and other possible causes of eosinophilia.
When diagnosed with HES, it is important to determine the extent of organ damage. A chest x-ray, pulmonary function tests, and echocardiogram are routinely performed to evaluate the heart and lungs. Other tests often performed in HES patients include liver and kidney function, creatine kinase, troponin, serum vitamin B12 levels, erythrocyte sedimentation rate (ESR), and serum tryptase levels.
Treatment of hypereosinophilic syndrome (HES):
The goal of HES treatment is to reduce eosinophil levels in the blood and tissues, thereby preventing tissue damage–especially in the heart. Standard HES treatment includes glucocorticosteroid medications such as prednisone for hypereosinophilia and often for ongoing treatment of organ damage, and chemotherapeutic agents such as hydroxyurea, chlorambucil, etoposide, cladribine, and vincristine to control eosinophil counts. Interferon-alpha may also be used as a treatment. This medication must be administered by frequent injections.
Research is uncovering new therapies for HES. One new approach for controlling malignant cell growth is the use of tyrosine kinase inhibitors such as GleevecTM (imatinib) for patients with the FIP1L1/PDGFRA-associated fusion gene or other similar gene fusions. Monoclonal antibody therapy, such as alemtuzumab (anti-CD52) has also shown promise for the treatment of HES. In fact, based on a recent phase III randomized, placebo-controlled trial, the monoclonal antibody Nucala or mepolizumab (anti-IL-5) has just received approval by the U.S. Food and Drug Administration for treatment of adults and children aged 12 years and older with HES for six months or longer without another identifiable non-blood-related cause of the disease.

Prednisone tablets commonly used as first-line therapy in hypereosinophilic syndrome to rapidly suppress eosinophilia and control organ-damaging inflammation
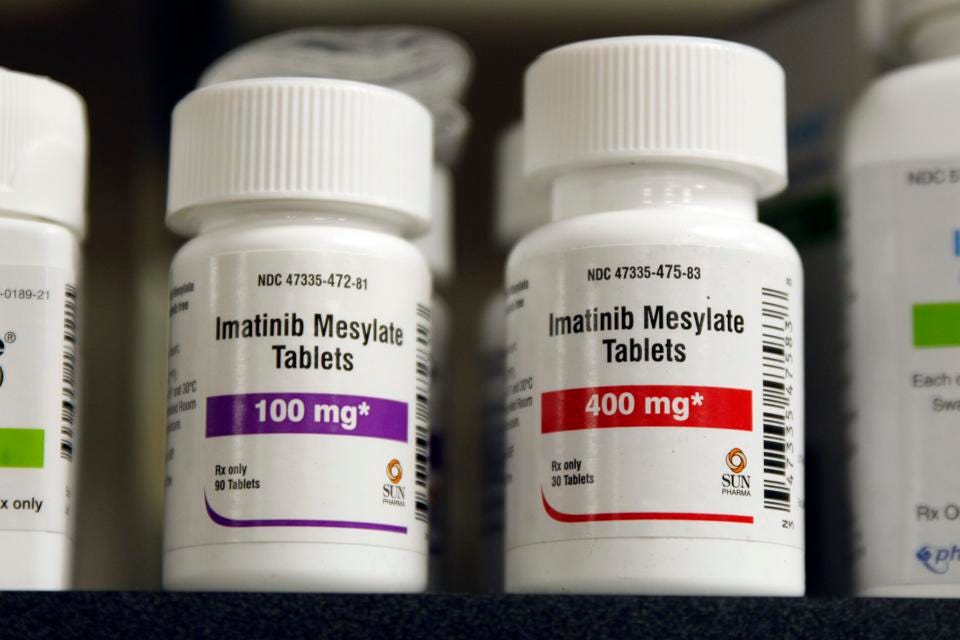
Imatinib mesylate tablets used in the treatment of hypereosinophilic syndrome, particularly in patients with PDGFRA or related tyrosine kinase rearrangements, demonstrating targeted molecular therapy
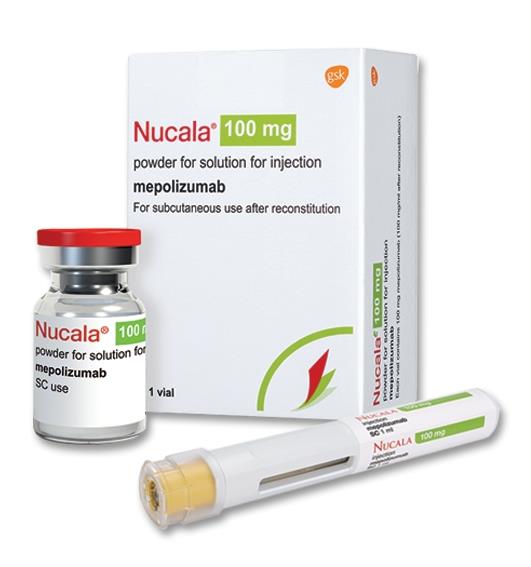
Mepolizumab (Nucala), an anti-IL-5 monoclonal antibody, used in the treatment of hypereosinophilic syndrome to reduce eosinophil levels and control disease activity in steroid-refractory or steroid-dependent patients
Treatments include immediate therapy, definitive therapies (treatments directed at the disorder itself), and supportive therapies.
Immediate therapy:
For patients with very severe eosinophilia, complications of hyperleukocytosis, or both (usually patients with eosinophilic leukemia), high-dose IV corticosteroids (eg, prednisone 1 mg/kg or equivalent) should be initiated as soon as possible. If the eosinophil count is much lower (eg, by ≥ 50%) after 24 hours, the corticosteroid dose can be repeated daily; if not, an alternative treatment (eg, hydroxyurea) is begun. Once the eosinophil count begins to decline and is under better control, additional drugs may be started.
Definitive therapy:
Patients with the FIP1L1/PDGFRA-associated fusion gene (or similar fusion genes) are usually treated with imatinib and, particularly if heart damage is suspected, corticosteroids. If imatinib is ineffective or poorly tolerated, another tyrosine kinase inhibitor (eg, dasatinib, nilotinib, sorafenib) can be used, or allogeneic hematopoietic stem cell transplantation can be used.
Patients without the FIP1L1/PDGFRA-associated fusion gene, even if asymptomatic, are often given one dose of prednisone 60 mg (or 1 mg/kg) orally to determine corticosteroid responsiveness (ie, a decrease in the eosinophil count). In patients with symptoms or organ damage, prednisone is continued at the same dose for 2 weeks, then tapered. Patients without symptoms and organ damage are monitored for at least 6 months for these complications. If corticosteroids cannot be easily tapered, a corticosteroid-sparing drug (eg, hydroxyurea, interferon alfa) can be used.
Supportive care:
Supportive drug therapy and surgery may be required for cardiac manifestations (eg, infiltrative cardiomyopathy, valvular lesions, heart failure). Thrombotic complications may require the use of antiplatelet drugs (eg, aspirin, clopidogrel, ticlopidine); anticoagulation is indicated if a left ventricular mural thrombus is present or if transient ischemic attacks persist despite the use of aspirin.
Investigational therapy:
Mepolizumab and other anti‐interleukin‐5 antibodies are investigational treatments for hypereosinophilic syndrome. Mepolizumab is a fully human monoclonal antibody against interleukin 5 (a regulator of eosinophil production). Mepolizumab decreases eosinophilia and the need for high-dose corticosteroid therapy and is currently available for compassionate use in the US for patients with refractory hypereosinophilic syndrome.
Prognosis of hypereosinophilic syndrome (HES):
The prognosis of HES depends upon the extent of any organ damage. In very severe cases, HES may be fatal, but there is hope. Survival rates have improved greatly. In 1975, only 12% of HES patients survived three years. Today, more than 80% of HES patients survive five years or more.
Death usually results from an organ, particularly the heart, dysfunction. Cardiac involvement is not predicted by the degree or duration of eosinophilia. The prognosis varies depending on the response to therapy. Response to imatinib improves the prognosis among patients with the FIP1L1/PDGFRA-associated fusion gene and other responsive gene fusions. Current therapy has improved the prognosis.
Summary:
Hypereosinophilic Syndrome (HES) is a rare hematologic disorder defined by persistent, unexplained eosinophilia, typically with an absolute eosinophil count exceeding 1.5 × 10⁹/L, leading to progressive organ damage due to eosinophil-mediated inflammation. Eosinophils are granulocytic white blood cells involved in immune responses, particularly in parasitic infections and allergic conditions; however, sustained eosinophil elevation in the absence of secondary causes raises concern for HES. Clinical manifestations vary widely and may involve the skin, heart, lungs, gastrointestinal tract, nervous system, and bone marrow, with cardiac involvement representing a major determinant of morbidity and mortality. Management of hypereosinophilic syndrome is individualized and aims to rapidly control eosinophil levels, prevent irreversible organ damage, and target underlying disease mechanisms. Therapeutic options include systemic corticosteroids as first-line therapy, molecularly targeted agents such as tyrosine kinase inhibitors for genetically defined subtypes, biologic therapies including anti–IL-5 monoclonal antibodies, immunomodulatory agents, and cytotoxic chemotherapy in selected cases, with stem cell transplantation reserved for aggressive or refractory disease. Given the diagnostic complexity and heterogeneity of HES, early recognition, comprehensive evaluation, and timely initiation of appropriate therapy are essential to improve long-term outcomes.
Questions and Answers:
What is hypereosinophilic syndrome?
Hypereosinophilic syndrome is a rare hematologic disorder characterized by persistent eosinophilia, typically an absolute eosinophil count exceeding 1.5 × 10⁹/L, associated with organ damage due to eosinophil infiltration and inflammation.
What causes hypereosinophilic syndrome?
Hypereosinophilic syndrome may be idiopathic or secondary to clonal myeloid disorders, aberrant T-cell proliferation, genetic tyrosine kinase rearrangements such as PDGFRA, or immune-mediated mechanisms.
How is hypereosinophilic syndrome diagnosed?
Diagnosis requires sustained eosinophilia, exclusion of secondary causes such as parasitic infection or drug reactions, and evidence of eosinophil-related organ involvement, supported by molecular and immunophenotypic testing.
What organs are commonly affected in hypereosinophilic syndrome?
The skin, heart, lungs, gastrointestinal tract, nervous system, and bone marrow are commonly involved, with cardiac disease being a major cause of morbidity and mortality.
What are the skin manifestations of hypereosinophilic syndrome?
Cutaneous involvement includes erythematous papules, plaques, urticaria-like eruptions, eczema-like rashes, and angioedema resulting from eosinophilic dermal infiltration.
How does hypereosinophilic syndrome affect the heart?
Cardiac involvement includes myocardial infiltration, endomyocardial fibrosis, mural thrombus formation, and restrictive cardiomyopathy, often detected by echocardiography or cardiac MRI.
What is the difference between myeloproliferative and lymphoproliferative hypereosinophilic syndrome?
The myeloproliferative variant is associated with clonal genetic abnormalities and responds to tyrosine kinase inhibitors, while the lymphoproliferative variant involves aberrant T cells and typically responds to corticosteroids.
Which genetic mutations are associated with hypereosinophilic syndrome?
Rearrangements involving PDGFRA, PDGFRB, FGFR1, or PCM1-JAK2 are characteristic of clonal myeloid hypereosinophilic syndromes and have important therapeutic implications.
What drugs can cause secondary eosinophilia?
Antibiotics, anticonvulsants, NSAIDs, ACE inhibitors, proton pump inhibitors, antimalarials, and sulfonamides are among the most common drug classes associated with eosinophilia.
What is the first-line treatment for hypereosinophilic syndrome?
Systemic corticosteroids are the first-line therapy in most patients, leading to rapid reduction in eosinophil counts and improvement of organ involvement.
When is imatinib used in hypereosinophilic syndrome?
Imatinib is used in patients with PDGFRA- or related tyrosine kinase–positive hypereosinophilic syndrome and often produces dramatic and sustained hematologic responses.
What is the role of mepolizumab in hypereosinophilic syndrome?
Mepolizumab, an anti-IL-5 monoclonal antibody, is effective in reducing eosinophil counts and steroid dependence in patients with refractory or relapsing hypereosinophilic syndrome.
Can hypereosinophilic syndrome progress to leukemia or lymphoma?
Yes, the myeloproliferative variant carries a risk of progression to acute myeloid or lymphoblastic leukemia, while the lymphoproliferative variant may evolve into T-cell lymphoma.
Is hypereosinophilic syndrome curable?
Some molecularly defined forms, particularly PDGFRA-positive disease, can achieve long-term remission with targeted therapy, while other forms require chronic disease control.
What investigations are essential in suspected hypereosinophilic syndrome?
Essential tests include peripheral blood smear, bone marrow examination, flow cytometry, molecular genetic testing, echocardiography, and targeted organ assessment.
References:
Jane Liesveld, James P. Wilmot. Hypereosinophilic Syndrome. MSD Manual Professional Edition – Hematology and Oncology.
https://www.msdmanuals.com/professional/hematology-and-oncology/eosinophilic-disorders/hypereosinophilic-syndrome
Apperley JF, Gardembas M, Melo JV, et al. Response to imatinib mesylate in patients with chronic myeloproliferative diseases with rearrangements of the platelet-derived growth factor receptor beta. New England Journal of Medicine. 2002;347:481–487.
Gotlib J. World Health Organization–defined eosinophilic disorders: 2017 update on diagnosis, risk stratification, and management. American Journal of Hematology. 2017;92:1243–1259.
Ogbogu PU, Bochner BS, Butterfield JH, et al. Hypereosinophilic syndromes: A multicenter, retrospective analysis of clinical characteristics and response to therapy. Journal of Allergy and Clinical Immunology. 2009;124:1319–1325.
Cortes J, Ault P, Koller C, et al. Efficacy of imatinib mesylate in the treatment of idiopathic hypereosinophilic syndrome. Blood. 2003;101:4714–4716.
Rothenberg ME, Klion AD, Roufosse FE, et al. Treatment of patients with the hypereosinophilic syndrome with mepolizumab. New England Journal of Medicine. 2008;358:1215–1228.
What causes secondary eosinophilia? Medscape.
https://www.medscape.com/answers/202030-115250/what-causes-secondary-eosinophilia
Eosinophilia. Wikipedia.
https://en.wikipedia.org/wiki/Eosinophilia
Hypereosinophilic syndrome. NIH – Genetic and Rare Diseases Information Center (GARD).
https://rarediseases.info.nih.gov/diseases/2804/hypereosinophilic-syndrome
Noh HR, Magpantay GG. Hypereosinophilic syndrome. Allergy and Asthma Proceedings. 2017;38(1):78–81.
Curtis C, Ogbogu P. Hypereosinophilic syndrome. Clinical Reviews in Allergy & Immunology. 2016;50(2):240–251.
Fiona Larsen. Hypereosinophilic Syndrome. DermNet NZ.
https://dermnetnz.org/topics/hypereosinophilic-syndrome
Venkata Anuradha Samavedi, MBBS, MD. Hypereosinophilic Syndrome. Medscape Reference. 2017.
https://emedicine.medscape.com/article/202030-overview
Idiopathic hypereosinophilic syndrome with Löeffler’s endocarditis. ResearchGate Scientific Figure.
https://www.researchgate.net/figure/Hypereosinophilic-syndrome-with-cardiac-involvement-in-our-patient-was-marked-by-a_fig2_263282480
Andrew Moore, MD. Hypereosinophilic Syndrome. American Academy of Allergy, Asthma & Immunology (AAAAI).
https://www.aaaai.org/Conditions-Treatments/Related-Conditions/hypereosinophilic-syndrome
Drug-induced eosinophilia.
https://diseasesandconditions.net/drug-induced-eosinophilia/
Roufosse FE, Kahn J-E, Rothenberg ME, et al. Efficacy and safety of mepolizumab in hypereosinophilic syndrome: A phase III randomized placebo-controlled trial. Journal of Allergy and Clinical Immunology. 2020. doi:10.1016/j.jaci.2020.08.037
Looman KIM, Nuver ME, Korevaar TIM, et al. Hypereosinophilic syndrome with multiorgan involvement: An interdisciplinary work-up. BMJ Case Reports CP. 2021;14:e240243.
Klion AD. How I treat hypereosinophilic syndromes. Blood. 2015;126(9):1069–1077.
Gotlib J. World Health Organization–defined eosinophilic disorders: 2015 update on diagnosis, risk stratification, and management. American Journal of Hematology. 2015;90(11):1077–1089.
Roufosse FE, Goldman M, Cogan E. Hypereosinophilic syndromes. Orphanet Journal of Rare Diseases. 2007;2:37.
Keywords:
hypereosinophilic syndrome, hypereosinophilic syndrome HES, hypereosinophilia, eosinophilia causes, persistent eosinophilia, eosinophil disorders, idiopathic hypereosinophilic syndrome, clonal hypereosinophilic syndrome, reactive hypereosinophilia, eosinophilia organ damage, hypereosinophilic syndrome diagnosis, hypereosinophilic syndrome treatment, HES management guidelines, HES prognosis, eosinophilic syndromes hematology, PDGFRA positive hypereosinophilic syndrome, PDGFRB rearrangement eosinophilia, FIP1L1-PDGFRA fusion, bone marrow eosinophilia, eosinophils peripheral blood smear, hypereosinophilic syndrome skin manifestations, cardiac involvement hypereosinophilic syndrome, Loeffler endocarditis eosinophilia, corticosteroids hypereosinophilic syndrome, imatinib hypereosinophilic syndrome, mepolizumab hypereosinophilic syndrome, biologic therapy eosinophilia, anti-IL-5 therapy HES, drug-induced eosinophilia, secondary eosinophilia causes, eosinophil count greater than 1.5 × 10⁹/L, rare hematologic disorders, eosinophilic leukemia differential diagnosis, Ask Hematologist, Dr Moustafa Abdou


Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now

I am a 37 year old female. I have been regularly donating plasma for almost two months now, but yesterday I was deferred because my hematocrit was at 35%. The nurse told me that this is still a healthy level, just too low to donate, but I am a little bewildered that this happened after I have donated at least a dozen times without incident. I was not currently on my period, and I had donated just two days prior just fine. Is there anything else besides an obvious injury that would cause a sudden drop in hematocrit? How can I reliably raise my levels before my next appointment?
Hi Erin,
Thank you for your comment.
As long as your other blood indices e.g. white cell count, hemoglobin, MCV, MCH, and platelets are fine, the low hematocrit could be caused by depleted iron stores.
I would suggest to check your serum iron, ferritin, B12, and folate.
BW,
If HES is a prothrombotic state which may get worse by corticosteroids,TKIs,So what is the pathobiology,clinical spectrum? Also;is there any role for Herdidary thrombophilia testing to guide primary or secondary thromboprohylaxis in HES?
Hi Sabry,
Thank you for your comment.
Yes, hypereosinophilic syndrome (HES) has been associated with a prothrombotic tendency. The increased levels of eosinophils in the blood can lead to endothelial damage and activation of clotting factors, contributing to a higher risk of thrombotic events. Additionally, eosinophils release various proinflammatory mediators that can further promote a prothrombotic state. Monitoring for thrombotic complications is important in the management of patients with hypereosinophilic syndrome, and anticoagulation may be considered in certain cases.
BW,
Dr M Abdou