Human Immunodeficiency Virus

Human Immunodeficiency Virus (HIV) – 3D structural model showing envelope glycoproteins and viral capsid.
Human Immunodeficiency Virus (HIV) is a major global health concern and remains one of the most significant infectious diseases affecting individuals, communities, and healthcare systems worldwide. HIV is a retrovirus that targets and progressively destroys CD4-positive T lymphocytes, leading to immune dysfunction and increased vulnerability to opportunistic infections and malignancies.
Following initial exposure, HIV infection often presents with a transient flu-like illness, after which patients typically enter a prolonged asymptomatic phase that may last for years. During this period, the virus continues to replicate and progressively impair immune function. HIV is most commonly transmitted through sexual contact, exposure to infected blood, and vertical transmission during pregnancy, childbirth, or breastfeeding. Without antiretroviral therapy (ART), persistent viral replication eventually leads to severe immunosuppression and the clinical development of Acquired Immunodeficiency Syndrome (AIDS).
AIDS represents the most advanced stage of HIV infection and is characterised by profound CD4+ lymphocyte depletion, chronic lymphadenopathy, and susceptibility to recurrent or severe opportunistic infections, including fungal infections, atypical mycobacteria, and Pneumocystis jirovecii pneumonia. The progressive decline in CD4 count is a hallmark of disease evolution and remains a key predictor of morbidity and mortality.
Clinical features:
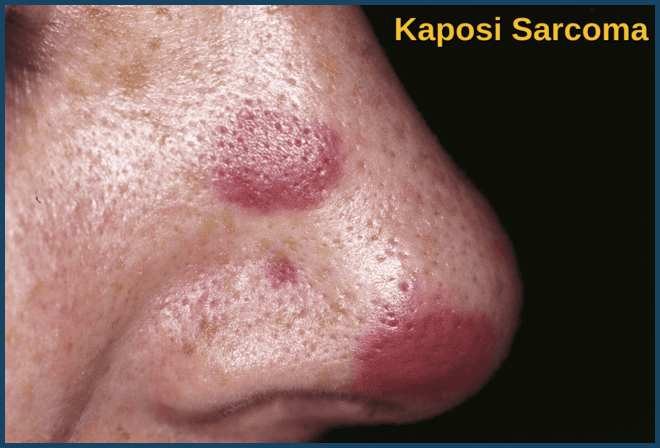
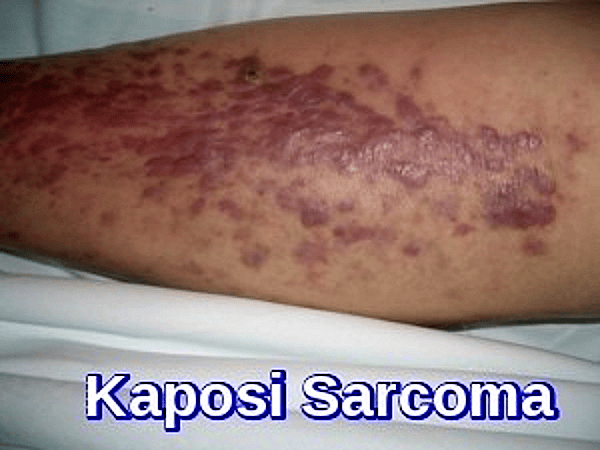
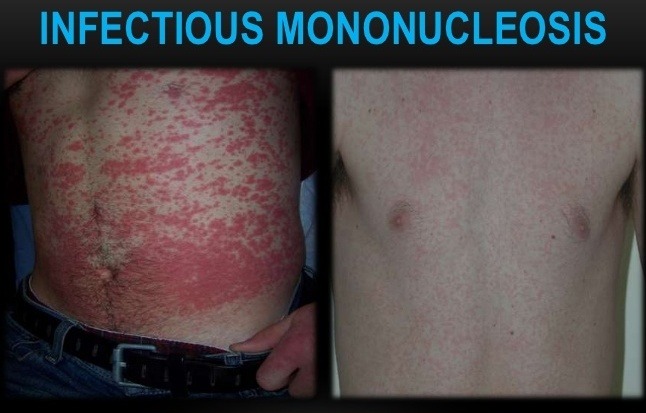
- A proportion of patients with HIV infection develop malignancies, particularly Kaposi’s sarcoma, aggressive non-Hodgkin’s lymphoma, and Hodgkin’s disease. The lymphomas frequently contain the EBV virus.
- Patients with acquired immunodeficiency syndrome (AIDS) are often anemic, and this can be exacerbated by treatment and cotrimoxazole (Septrin) used in prophylaxis for pneumocystis.
- The neutrophil count may be reduced; in some cases, this deficiency is autoimmune. Immune thrombocytopenia is more common and may necessitate splenectomy.

AIDS – hypercellular dysplastic bone marrow with multilineage abnormalities common in advanced HIV infection.
- The bone marrow in AIDS patients displays non-specific abnormalities, including hypercellularity, megaloblastic erythropoiesis, myeloid dysplasia, lymphoid aggregates, eosinophilia, plasmacytosis, and increased reticulin.
Diagnosis:
Screening for human immunodeficiency virus (HIV) infection is paramount since infected individuals may remain asymptomatic for years while the infection progresses.
- A standard serological test diagnoses HIV infection, and progression can be monitored by regular measurement of CD4+ cells in the blood.
- Secondary testing that may be performed to assist with diagnosis or staging includes viral culture, lymph node biopsy, viral DNA polymerase chain reaction (PCR), and genotyping of viral DNA/RNA.
- In the presence of fever, thorough clinical examination and detailed investigations must be conducted to find the cause.
- A bone marrow examination may occasionally be the most direct way to detect mycobacterial infections and lymphomas.
Treatment:
Understanding the structure, replication cycle, and immune-evasion mechanisms of the Human Immunodeficiency Virus (HIV) is essential for developing effective treatment and prevention strategies. Modern HIV therapy focuses on suppressing viral replication, restoring immune function, and minimising the risk of opportunistic infections.
The management of HIV depends on the stage of infection, the patient’s immunological status, and the presence of opportunistic or coexisting infections. The fundamental objective is to prevent progressive immune deterioration and reduce the likelihood of AIDS-defining illnesses. The cornerstone of HIV treatment is antiretroviral therapy (ART), which uses a combination of antiretroviral (ARV) drugs to achieve sustained viral suppression and halt disease progression. ART has transformed HIV into a chronic, manageable condition and significantly reduced HIV-related morbidity, mortality, and transmission.
ART regimens typically combine agents from different drug classes to maximally inhibit viral replication. Effective treatment leads to undetectable viral loads, recovery of CD4 T-cell numbers, and improved immune resilience. Early initiation of ART is associated with superior long-term outcomes. The World Health Organization (WHO) recommends offering ART to all individuals diagnosed with HIV, regardless of CD4 count, to optimise clinical outcomes and reduce transmission risk.
Preventive strategies remain an integral part of HIV care. Prophylaxis against specific opportunistic infections is indicated when CD4 counts fall below defined thresholds. In addition, pre-exposure prophylaxis (PrEP) is recommended for individuals at substantial risk of acquiring HIV and is highly effective when taken consistently. Many countries have incorporated WHO guidelines into national protocols to broaden access to ART and PrEP and improve overall HIV prevention efforts.
Successful, sustained ART not only suppresses viral replication but also promotes gradual immune reconstitution, reflected by rising CD4 T-cell numbers and improved host defences. Continuous adherence, regular monitoring, and management of comorbidities are essential to maintaining long-term treatment success.
Key Facts:
*HIV remains a major global public health issue, having claimed 40.4 million [32.9–51.3 million] lives so far, with ongoing transmission in all countries globally, with some countries reporting increasing trends in new infections when previously on the decline.
*There is no cure for HIV infection. However, with access to effective HIV prevention, diagnosis, treatment and care, including for opportunistic infections, HIV infection has become a manageable chronic health condition, enabling people living with HIV to lead long and healthy lives.
*By 2025, 95% of all people living with HIV (PLHIV) should have a diagnosis, 95% of those should be taking lifesaving antiretroviral treatment (ART), and 95% of PLHIV on treatment should achieve a suppressed viral load for the benefit of the person’s health and for reducing onward HIV transmission.
Summary:
Human Immunodeficiency Virus (HIV) is a globally significant retroviral infection that targets CD4 T lymphocytes, progressively weakening the immune system and predisposing affected individuals to opportunistic infections and malignancies. HIV is primarily transmitted through sexual contact, exposure to infected blood, and vertical transmission during pregnancy, childbirth, or breastfeeding. Without treatment, persistent viral replication leads to severe immunosuppression and the development of Acquired Immunodeficiency Syndrome (AIDS). Modern antiretroviral therapy (ART) suppresses viral replication, restores immune function, prevents disease progression, and eliminates onward transmission when viral load becomes undetectable. Current WHO guidelines recommend initiating ART immediately after diagnosis and offering pre-exposure prophylaxis (PrEP) to individuals at substantial risk. With early diagnosis, consistent ART, and appropriate prophylaxis for opportunistic infections, people living with HIV can achieve long-term viral suppression and lead healthy, productive lives. Despite major advances, HIV remains a major public health challenge worldwide, underscoring the need for ongoing prevention, testing, and equitable access to treatment.
Questions and Answers:
What is Human Immunodeficiency Virus (HIV)?
HIV is a retrovirus that targets CD4-positive T lymphocytes, leading to progressive immune suppression and increased vulnerability to opportunistic infections if left untreated.
How is HIV transmitted?
HIV is transmitted through unprotected sexual contact, exposure to infected blood, and vertical transmission during pregnancy, childbirth, or breastfeeding.
What are the early symptoms of HIV infection?
Many patients experience a transient flu-like illness during acute infection, followed by a prolonged asymptomatic period while the virus continues to replicate and damage CD4 T cells.
What does HIV do to the immune system?
HIV progressively depletes CD4+ lymphocytes, causing immune dysfunction that leads to recurrent infections, chronic lymphadenopathy, and susceptibility to atypical organisms.
What is the difference between HIV and AIDS?
HIV is the viral infection itself, while AIDS represents the most advanced stage, defined by severe CD4 depletion and the presence of opportunistic infections or AIDS-defining illnesses.
How is HIV diagnosed?
HIV is diagnosed using serological tests such as antigen/antibody combination assays, confirmed by supplemental testing and supported by viral load and CD4 count measurements.
What is antiretroviral therapy (ART)?
ART is a combination of antiretroviral drugs designed to suppress viral replication, restore immune function, and prevent progression to AIDS. It is recommended for all patients immediately after diagnosis.
How does ART improve long-term outcomes in HIV?
Successful ART achieves sustained viral suppression, gradually increases CD4 T-cell counts, reduces opportunistic infections, and significantly lowers HIV-related morbidity and mortality.
What are opportunistic infections associated with HIV/AIDS?
Common opportunistic infections include Pneumocystis jirovecii pneumonia, fungal infections, atypical mycobacteria, and viral reactivations, occurring due to profound immune suppression.
What is Kaposi Sarcoma in HIV patients?
Kaposi Sarcoma is an HHV-8–associated malignancy presenting as violaceous skin lesions, often on the face or lower limbs, and is strongly linked to advanced HIV infection.
What does AIDS-related bone marrow involvement look like?
AIDS bone marrow may show hypercellularity with multilineage dysplasia, reflecting chronic viral impact, opportunistic infections, and drug-related marrow suppression.
Can HIV be cured?
There is currently no cure for HIV, but effective ART allows individuals to live long, healthy lives with undetectable viral loads and significantly reduced transmission risk.
What prevention strategies reduce HIV transmission?
Key preventive measures include ART, condom use, harm reduction for blood exposure, pre-exposure prophylaxis (PrEP), and prevention of vertical transmission during pregnancy.
What are the WHO 95-95-95 HIV targets?
The 95-95-95 goals aim for: 95% of people with HIV diagnosed, 95% of those on ART, and 95% achieving viral suppression to reduce illness and prevent onward transmission.
References:
U.S. Preventive Services Task Force. Screening for HIV. Available at: http://www.uspreventiveservicestaskforce.org/uspstf/uspshivi.htm. Accessed June 16, 2011.
Sharp PM, Hahn BH. Origins of HIV and the AIDS pandemic. Cold Spring Harbor Perspectives in Medicine. 2011;1(1):a006841. doi:10.1101/cshperspect.a006841.
Kaposi’s sarcoma. Wikipedia. Available at: https://en.wikipedia.org/wiki/Kaposi%27s_sarcoma#cite_note-1
Sand M, Sand D, Thrandorf C, Paech V, Altmeyer P, Bechara FG. Cutaneous lesions of the nose. Head & Face Medicine. 2010;6:7. doi:10.1186/1746-160X-6-7.
Branson BM, Handsfield HH, Lampe MA, et al. Revised recommendations for HIV testing of adults, adolescents, and pregnant women in health-care settings. MMWR Recommendations and Reports. 2006;55:1–17.
Mayo Clinic. HIV/AIDS – Symptoms and causes. Available at: https://www.mayoclinic.org/diseases-conditions/hiv-aids/symptoms-causes/syc-20373524
Africa CDC. HIV (Human Immunodeficiency Virus). Available at: https://africacdc.org/disease/hiv-human-immunodeficiency-virus/
World Health Organization (WHO). HIV and AIDS. Available at: https://www.who.int/news-room/fact-sheets/detail/hiv-aids
Keywords:
Human Immunodeficiency Virus, HIV infection, AIDS disease, HIV symptoms, HIV diagnosis, HIV treatment, antiretroviral therapy ART, CD4 T helper cells, HIV viral load, HIV opportunistic infections, Kaposi Sarcoma HIV, AIDS bone marrow changes, HIV skin lesions, HIV transmission routes, HIV prevention strategies, PrEP HIV prevention, PEP HIV exposure, WHO HIV guidelines, HIV testing recommendations, HIV global statistics, HIV epidemiology, HIV staging, HIV acute infection, HIV chronic infection, HIV/AIDS clinical features, HIV immune system damage, HIV progression, HAART therapy, HIV patient management, AskHematologist HIV


Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now