Infectious Mononucleosis
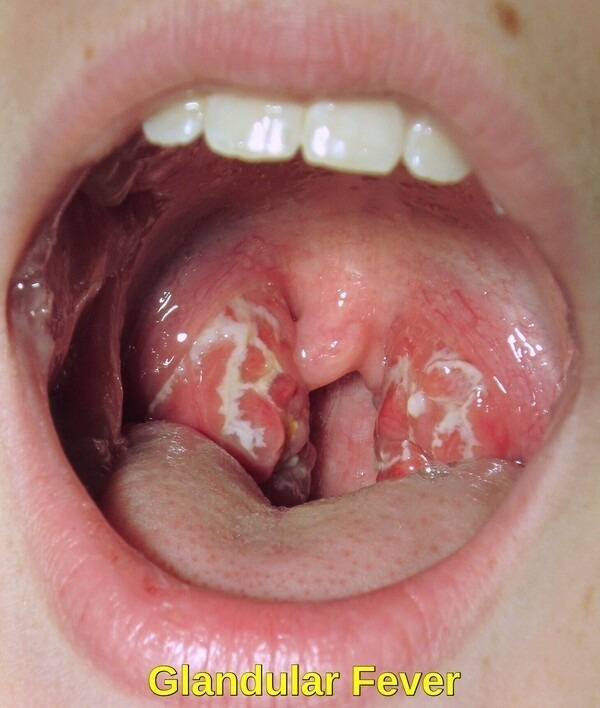
Exudative tonsillitis in infectious mononucleosis (glandular fever), showing swollen erythematous tonsils with white patches.
Infectious Mononucleosis (Glandular Fever)—commonly referred to as mono—is an acute viral illness caused predominantly by the Epstein–Barr virus (EBV), a member of the herpesvirus family. First characterised in the 1920s, the infection is transmitted primarily through saliva, earning it the nickname “the kissing disease”, although sharing drinking glasses, utensils, or toothbrushes can also facilitate spread.
The incubation period ranges from four to eight weeks, and the condition most frequently affects adolescents and young adults. From a haematological perspective, infectious mononucleosis is clinically significant due to the diagnostic challenges it may pose, particularly when differentiating it from other causes of lymphadenopathy, atypical lymphocytosis, and pharyngitis.
While mono is usually self-limiting and not severe, patients may develop secondary infections such as streptococcal pharyngitis, sinusitis, or bacterial tonsillitis, which may complicate the clinical picture.
Clinical features:
- The disease may cause non-specific malaise, fever, sore throat, headaches, and lymphadenopathy (glandular fever); some cases are asymptomatic. Lymphadenopathy is almost universal, and it lasts for 1-2 weeks.
- The spleen is often palpable and there may be hepatomegaly and jaundice.
- Skin rashes are frequent. A macular erythematous rash may occur in patients with mono who are treated with ampicillin or amoxicillin.
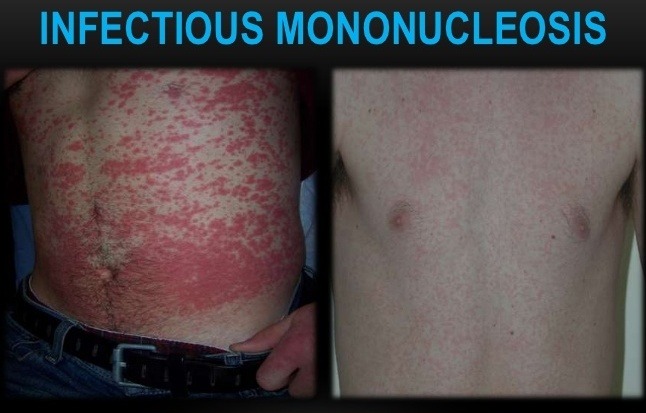
Characteristic amoxicillin-associated rash in a patient with infectious mononucleosis, showing widespread erythematous maculopapular exanthem.
A lymphocytosis develops and atypical mononuclear cells are found. These cells have irregular nuclei, often with nucleoli, but usually with condensed chromatin to distinguish them from blast cells. These cells are activated (reactive) T cells.
- Autoimmune hemolytic anemia or thrombocytopenia may also occur.
- N.B. Atypical mononuclear cells are also seen in other infections including cytomegalovirus (CMV) and toxoplasmosis.

Atypical lymphocytes seen in infectious mononucleosis, characterised by enlarged nuclei and abundant basophilic cytoplasm.
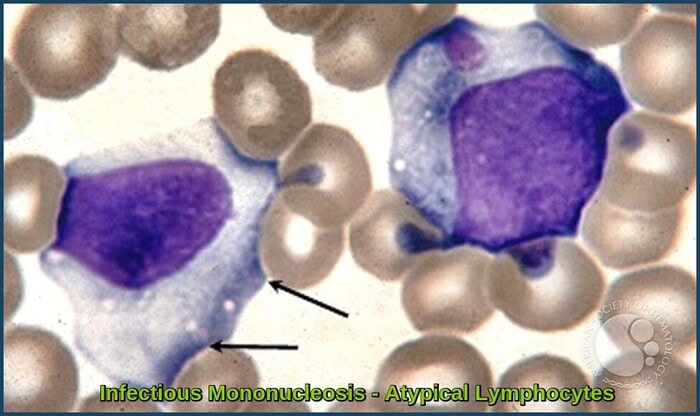
Large irregular atypical lymphocytes seen in the peripheral blood in infectious mononucleosis, showing cytoplasmic indentation by surrounding red blood cells that produces the classic “Dutch skirt” appearance.
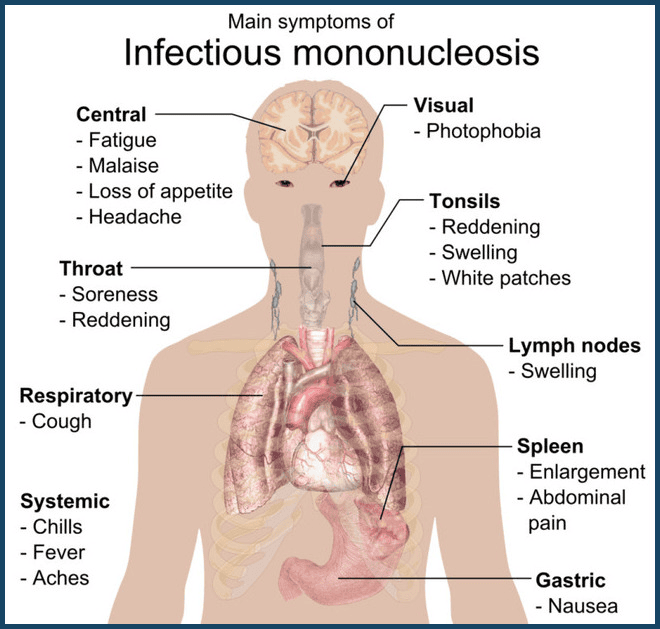
Infographic summarising the key clinical symptoms of infectious mononucleosis, including fatigue, sore throat, swollen tonsils, lymphadenopathy, fever, and splenomegaly.
Diagnosis:
- The diagnosis of EBV infection is dependent on the demonstration of agglutinins to horse or sheep red cells (Paul-Bunnell test).
- The mononuclear spot test or monospot test, a form of the heterophile antibody test, is a rapid test for infectious mononucleosis due to Epstein–Barr virus (EBV). It is an improvement on the Paul-Bunnell test.
Monospot Test Explained | Rapid Diagnosis of Infectious Mononucleosis (EBV)
- Although virtual 100% specificity exists with the Monospot test, rarely, other disorders have been reported that may produce a false-positive Monospot test result. These causes of false-positive Monospot test results include toxoplasmosis, rubella, systemic lupus erythematosus, and certain malignancies, particularly leukemias and/or lymphomas.
Treatment:
- The most effective treatment for the glandular fever is REST and drinking plenty of fluids, followed by a gradual return to normal activities. If the spleen is enlarged, all contact sports should be avoided until the enlargement has subsided completely.
- Closely monitor patients with extreme tonsillar enlargement for airway obstruction. Steroids are indicated for impending or established airway obstruction in individuals with Epstein-Barr virus (EBV) infectious mononucleosis.
- Surgery is necessary for spontaneous splenic rupture, which occurs in rare patients with EBV infectious mononucleosis and may be the initial manifestation of the condition.
- No effective antiviral therapy is available for Epstein-Barr virus (EBV) infectious mononucleosis in immunocompetent persons. Acyclovir and ganciclovir may reduce EBV shedding but are ineffective clinically.
- Treatment of immunocompromised patients with EBV lymphoproliferative disease is controversial. Acyclovir has not been proven to be beneficial.
- Short courses of corticosteroids are indicated for EBV infectious mononucleosis with hemolytic anemia, thrombocytopenia, CNS involvement, or extreme tonsillar enlargement. However, corticosteroids are not indicated for uncomplicated EBV infectious mononucleosis. Corticosteroids should be considered in those with impending airway obstruction.
- Patients with EBV infectious mononucleosis who have positive throat cultures for group A streptococci should not be treated because this represents colonization rather than infection.
- Treatment of group A streptococcal oropharyngeal colonization in patients with EBV infectious mononucleosis may result in a maculopapular rash.
Summary:
Infectious Mononucleosis (Glandular Fever) is an acute viral illness caused by the Epstein–Barr virus (EBV), characterised by fever, sore throat, lymphadenopathy and the presence of atypical lymphocytes on blood film. The infection is typically transmitted through saliva, with an incubation period of four to eight weeks, and most commonly affects adolescents and young adults. Clinical features include pharyngitis, tonsillar swelling with exudates, fatigue, splenomegaly, and occasionally a widespread rash—particularly following exposure to amoxicillin. Diagnosis is supported by heterophile antibody testing (Monospot test) and EBV serology, alongside haematological findings such as lymphocytosis and reactive lymphocytes. Although usually self-limiting, infectious mononucleosis may be complicated by secondary bacterial infections, airway obstruction, hepatitis, or splenic enlargement requiring activity restriction. Understanding the presentation, diagnostic challenges, and management strategy is essential for clinicians evaluating patients with suspected EBV infection.
Questions and Answers:
What is infectious mononucleosis and what causes it?
Infectious mononucleosis is an acute viral illness caused mainly by the Epstein–Barr virus (EBV), presenting with fever, sore throat, fatigue, lymphadenopathy, and atypical lymphocytosis.
How is infectious mononucleosis transmitted?
The infection spreads primarily through saliva—via kissing, shared drinking glasses, or toothbrushes—although close contact and respiratory secretions may also contribute.
What are the key symptoms of infectious mononucleosis?
Common symptoms include marked fatigue, fever, sore throat, swollen tonsils with exudates, cervical lymphadenopathy, splenomegaly, and a maculopapular rash, especially after amoxicillin exposure.
What are atypical lymphocytes and why are they seen in infectious mononucleosis?
Atypical lymphocytes are reactive T cells produced in response to EBV infection; they appear large with irregular nuclei and abundant cytoplasm and are a hallmark of infectious mononucleosis.
What does the “Dutch skirt” appearance of atypical lymphocytes mean?
The “Dutch skirt” appearance refers to cytoplasmic indentation of atypical lymphocytes by adjacent red cells, creating a frilled border characteristic of EBV-related reactive lymphocytosis.
How is infectious mononucleosis diagnosed?
Diagnosis is based on clinical features, lymphocytosis with atypical lymphocytes on blood film, a positive Monospot test detecting heterophile antibodies, and confirmatory EBV serology when needed.
How accurate is the Monospot test for EBV?
The Monospot test is highly specific but less sensitive in early infection and in young children, where false-negative results are more common, making EBV serology useful for confirmation.
Why does a rash occur after taking amoxicillin in infectious mononucleosis?
Up to 90% of patients with infectious mononucleosis develop a diffuse maculopapular rash after receiving amoxicillin due to a characteristic drug–virus interaction, not a true allergy.
Who is most likely to develop infectious mononucleosis?
Adolescents and young adults are most commonly affected, although EBV infection can occur at any age, often asymptomatically in childhood.
What complications can occur in infectious mononucleosis?
Potential complications include splenomegaly with risk of rupture, airway obstruction from tonsillar hypertrophy, secondary bacterial infections, hepatitis, and prolonged post-viral fatigue.
How long does infectious mononucleosis last?
Acute symptoms typically last 2–4 weeks, but fatigue and lymphadenopathy may persist for several additional weeks.
Can patients with infectious mononucleosis participate in sports?
Patients should avoid contact sports for at least 3–4 weeks due to the risk of splenic rupture associated with splenomegaly.
Is infectious mononucleosis contagious?
Yes. EBV remains present in saliva during active illness, and patients may continue shedding the virus for months after recovery.
What does infectious mononucleosis look like on a blood film?
Blood film findings show large reactive atypical lymphocytes with irregular nuclear contours and basophilic cytoplasm, sometimes demonstrating the classic “Dutch skirt” indentation.
What tonsillar findings suggest infectious mononucleosis?
Exudative tonsillitis with significant swelling, erythema, and white plaques is common, often resembling streptococcal pharyngitis but accompanied by marked fatigue and lymphocytosis.
References:
Ali J. Spontaneous rupture of the spleen in patients with infectious mononucleosis. Can J Surg. 1993 Feb;36(1):49–52.
Al-Jitawi SA, Hakooz BA, Kazimi SM. False positive Monospot test in systemic lupus erythematosus. Br J Rheumatol. 1987 Feb;26(1):71.
Bonoan JT, Cunha BA. Lymphoma vs. Monospot-negative EBV infectious mononucleosis. Infect Dis Pract. 1998;22:63–64.
Hoover K, Higginbotham K. Epstein–Barr Virus. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. Updated 2023 Aug 8. Main symptoms of infectious mononucleosis. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559285/figure/article-21268.image.f1/
Maslak P, McKenzie S. Infectious Mononucleosis. ASH Image Bank. Available from: https://imagebank.hematology.org/image/1867/infectious-mononucleosis–1
Bender CE. The value of corticosteroids in the treatment of infectious mononucleosis. JAMA. 1967 Feb 20;199(8):529–531.
Tynell E, Aurelius E, Brandell A, et al. Acyclovir and prednisolone treatment of acute infectious mononucleosis: A multicenter, double-blind, placebo-controlled study. J Infect Dis. 1996 Aug;174(2):324–331.
Cafasso J, Sanyal S, MD. Infectious Mononucleosis. Healthline. Available from: https://www.healthline.com/health/mononucleosis
Keywords:
infectious mononucleosis, glandular fever, Epstein–Barr virus, EBV infection, monospot test, heterophile antibodies, atypical lymphocytes, Dutch skirt lymphocytes, EBV rash amoxicillin, exudative tonsillitis, cervical lymphadenopathy, splenomegaly, mononucleosis diagnosis, EBV serology, monospot false negative, infectious mononucleosis complications, EBV treatment, mononucleosis blood film, EBV atypical lymphocytosis, amoxicillin rash mononucleosis, infectious mononucleosis symptoms, mononucleosis management, EBV tonsillitis, spontaneous splenic rupture, mononucleosis steroid use, EBV fatigue, glandular fever clinical features, EBV haematology findings


Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now

thanks for valuable medical information
but i deal with mono and hematology (CBC of mono patient) other than,Lymphocytosis
Hi Reda,
Thank you for your comment.
The CBC count is more useful in ruling out other diagnoses that may mimic infectious mononucleosis than in providing any specific diagnostic information. Because leukocytosis is the rule in infectious mononucleosis, the presence of a normal or decreased WBC count should suggest an alternative diagnosis. Lymphocytosis accompanies infectious mononucleosis, increases during the first few weeks of illness, and then gradually returns to normal.
BW,