Trypanosomiasis
Trypanosomiasis, also known as sleeping sickness or Chagas disease, is a vector-borne parasitic infection caused by protozoa of the genus Trypanosoma. It affects both humans and animals and is transmitted primarily through the bite of infected tsetse flies (Glossina species) in Africa or by triatomine (kissing) bugs in the Americas. The African form is caused by Trypanosoma brucei gambiense (West and Central Africa) and Trypanosoma brucei rhodesiense (East Africa), while the American form (Chagas disease) results from Trypanosoma cruzi infection. African trypanosomiasis typically progresses from a hemolymphatic phase—fever, lymphadenopathy, and malaise—to a neurological stage marked by sleep disturbances and cognitive impairment. In contrast, Chagas disease can lead to chronic cardiac and gastrointestinal complications years after the initial infection. Both forms remain major neglected tropical diseases, with early diagnosis and treatment crucial to preventing severe and potentially fatal outcomes.
American trypanosomiasis, also known as Chagas disease, affects millions of people throughout the Americas.
Carlos Chagas first described this disease in 1911 when he discovered the parasite in the blood of a Brazilian child with fever, lymphadenopathy, and anemia.
Trypanosoma cruzi, a protozoan hemoflagellate, is the parasite that causes this disease.
When humans are infected, the parasite can cause acute illness; however, the infection is generally asymptomatic. In some cases, usually many years after initial infection, the affected individual can have clinical signs and symptoms from damage to the heart or GI tract.
The disease is the leading cause of non-ischemic congestive heart failure worldwide and notably in Latin America where it is endemic.
Chagas disease can be treated with benznidazole or nifurtimox to kill the parasite. Both medicines are fully effective in curing the disease if given soon after infection at the onset of the acute phase, including cases of congenital transmission. The efficacy of both diminishes; however, the longer a person is infected, the more adverse reactions are more frequent at older age. Treatment is also indicated for those in whom infection has been reactivated (for example, due to immunosuppression) and for patients during the early chronic phase, including girls and women of childbearing age (before or after pregnancy) to prevent congenital transmission.
Human African trypanosomiasis, or sleeping sickness, is caused by infection with parasites of the genus Trypanosoma, transmitted by the tsetse fly.
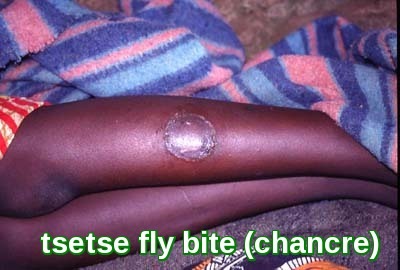
The tsetse fly bite erupts into a red chancre sore and within a few weeks, the person can experience fever, enlarged lymph nodes, hematuria, aching muscles and joints, headaches and irritability.
In the first phase, the patient has only intermittent bouts of fever with lymphadenopathy together with other non-specific signs and symptoms.
The second stage of the disease is marked by the involvement of the central nervous system with extensive neurological effects like changes in personality, alteration of the biological clock (the circadian rhythm), confusion, slurred speech, seizures and difficulty in walking and talking.
These problems can develop over many years and if not treated, the person dies. It is common to the African continent.
The disease has two forms, Trypanosoma brucie (T b) rhodesiense and T b gambiense; and is almost always fatal if untreated.
Despite a recent reduction in the number of reported cases, patients with African trypanosomiasis continue to present major challenges to clinicians. Because treatment for CNS-stage disease can be very toxic, diagnostic staging to distinguish early-stage from late-stage disease when the CNS invaded is crucial but remains problematic.
Diagnosis:
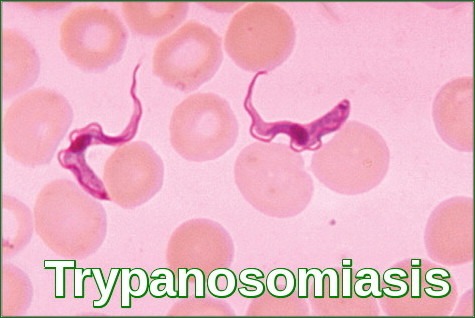
A key step in diagnosing trypanosomiasis is the direct detection of Trypomastigote forms of the parasite in peripheral blood smears, which appear as elongated flagellated organisms and are pathognomonic of infection. In the African variant (commonly African trypanosomiasis caused by Trypanosoma brucei gambiense or Trypanosoma brucei rhodesiense), the classic early clinical sign is Winterbottom’s sign—painless enlargement of the posterior cervical lymph nodes in the posterior triangle of the neck. In the American form (Chagas disease, due to Trypanosoma cruzi), one characteristic finding is Romana’s sign—unilateral periorbital oedema or conjunctival injection occurring at the site of parasite entry, often via a triatomine bug bite near the eye. Together, microscopic visualization of trypomastigotes and recognition of these eponymous signs guide early diagnosis and prompt management.
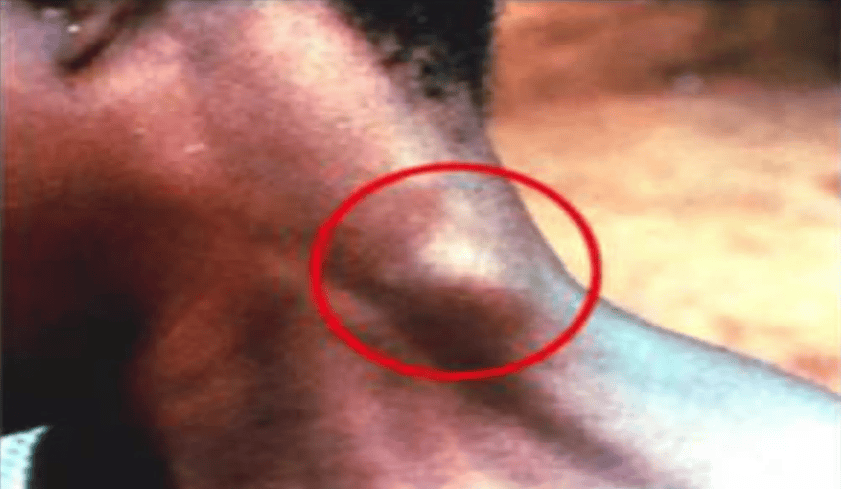
Winterbottom’s Sign: Swollen posterior cervical lymph nodes (adenopathy) are a classic early sign of the hemolymphatic phase of African Trypanosomiasis (Sleeping Sickness).
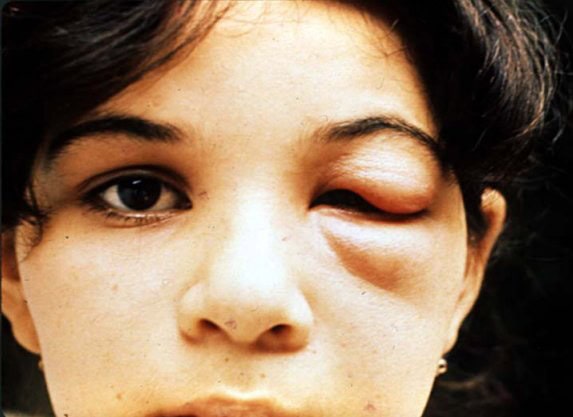
Romaña’s Sign: Unilateral swelling of the eyelid and surrounding tissue at the site where the Trypanosoma cruzi-carrying triatomine bug inoculated the parasite, characteristic of acute Chagas disease (American Trypanosomiasis).
Treatment:
Melarsoprol is the only available treatment for late-stage T b rhodesiense infection but can be lethal to 5% of patients owing to post-treatment reactive encephalopathy. Eflornithine combined with nifurtimox is the first-line treatment for late-stage T b gambiense.
Pentamidine and suramin are used in the first or early stage of T.b.gambiense and T.b. rhodesiense infections respectively.
New drugs are in the pipeline for the treatment of CNS human African trypanosomiasis, giving rise to cautious optimism.
Prevention:
Trypanosomiasis prevention primarily involves controlling the tsetse fly population, using insecticides to kill the flies, and avoiding exposure to their bites. Additionally, screening blood donors and implementing measures to prevent transmission through blood transfusions and organ transplants are important strategies in endemic areas. Early diagnosis and prompt treatment are crucial for improving outcomes and preventing the spread of the disease.
References:
World Health Organization (WHO). Trypanosomiasis (sleeping sickness and Chagas disease) – Key facts. Updated 2024. https://www.who.int/health-topics/trypanosomiasis
World Health Organization (WHO). Chagas disease (American trypanosomiasis) – Fact sheet. Updated 2024. https://www.who.int/news-room/fact-sheets/detail/chagas-disease-(american-trypanosomiasis)
World Health Organization (WHO). Human African trypanosomiasis – Symptoms, diagnosis, and treatment. https://www.who.int/trypanosomiasis_african/diagnosis/en/
Centers for Disease Control and Prevention (CDC). Parasites – African Trypanosomiasis (Sleeping Sickness). Updated 2024. https://www.cdc.gov/parasites/sleepingsickness
Centers for Disease Control and Prevention (CDC). Parasites – American Trypanosomiasis (Chagas Disease). Updated 2024. https://www.cdc.gov/parasites/chagas
U.S. National Institutes of Health (NIH) / National Library of Medicine (MedlinePlus). African Trypanosomiasis and Chagas Disease. https://medlineplus.gov/trypanosomiasis.html
Pan American Health Organization (PAHO). Chagas Disease – Epidemiological Update. 2024. https://www.paho.org/en/topics/chagas-disease
U.S. Department of Health and Human Services (HHS). Global Health – Neglected Tropical Diseases Initiative. https://www.hhs.gov
Bern C. Chagas’ Disease (American Trypanosomiasis). N Engl J Med. 2015;373(5):456–466.
Kennedy PGE. Clinical features, diagnosis, and treatment of human African trypanosomiasis (sleeping sickness). Lancet Neurol. 2013;12(2):186–194.
Ghaneim M. “African Trypanosoma.” Slideshare. Uploaded by MontasirGhaneim1. Available at: https://www.slideshare.net/slideshow/african-trypanosoma/235437979
Nguyen T., Waseem M. (2023). Chagas Disease. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459272/
Keywords:
trypanosomiasis, sleeping sickness, Chagas disease, African trypanosomiasis, American trypanosomiasis, Trypanosoma brucei, Trypanosoma cruzi, Trypanosoma brucei gambiense, Trypanosoma brucei rhodesiense, tsetse fly, triatomine bug, vector-borne parasitic infection, parasitic disease Africa, Chagas disease heart complications, neurological sleeping sickness, hemolymphatic phase, neglected tropical diseases, parasitic infection diagnosis, tropical medicine, Ask Hematologist, Dr Moustafa Abdou, trypomastigotes, Winterbottom’s sign, Romanã’s sign

Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now