Thrombotic Disorders

Gross pathological specimen demonstrating renal vein thrombosis with occlusion of the renal vein and secondary renal congestion
Thrombotic disorders, including venous thrombosis, arterial thrombosis, and hypercoagulable states, are increasingly encountered in clinical practice. Hematologists play a central role in the diagnosis and management of patients presenting with blood clots, such as deep vein thrombosis (DVT) and pulmonary embolism (PE). Major advances in our understanding of hypercoagulability and thrombophilia have improved risk stratification, diagnostic evaluation, and the development of targeted antithrombotic therapies.
Thrombosis is the formation of a blood clot inside a blood vessel, obstructing blood flow through the circulatory system. When a blood vessel is injured, the body uses platelets and fibrin to form a blood clot to prevent blood loss. Even when a blood vessel is not injured, blood clots may form in the body under certain conditions. A clot, or a piece of the clot, that breaks free and begins to travel around the body is known as an embolus.

Clinical photograph demonstrating unilateral leg swelling and erythema consistent with deep vein thrombosis (DVT)
In healthy people, a homeostatic balance exists between procoagulant (clotting) forces and anticoagulant and fibrinolytic forces. Numerous genetic, acquired, and environmental factors can tip the balance in favour of coagulation, leading to the pathologic formation of thrombi in veins (e.g. deep venous thrombosis [DVT]), arteries (e.g. myocardial infarction, ischemic stroke), or cardiac chambers. Thrombi can obstruct blood flow at the site of formation or detach and embolize to block a distant blood vessel (e.g. pulmonary embolism, embolic stroke).
It is now recognised that most, if not all, patients with venous thromboembolism have a genetic basis for the disorder (“thrombophilia“).
Clinical episodes of thrombosis are precipitated by acquired thrombogenic triggers, which may be overt (e.g., pregnancy) or subclinical.
Aetiology:
Genetic defects that increase the propensity for venous thromboembolism (VTE) include:
Factor V Leiden mutation:
Factor V Leiden mutation causes resistance to activated protein C (APC).
Mutations of factor V make it resistant to its normal cleavage and inactivation by activated protein C and predispose to venous thrombosis.
Activated protein C (APC), in complex with protein S, degrades coagulation factors Va and VIIIa, thus inhibiting coagulation.
Any of several mutations to factor V make it resistant to inactivation by APC, increasing the tendency for thrombosis. Factor V Leiden is the most common of these mutations. Homozygous mutations increase the risk of thrombosis more than do heterozygous mutations. Still, it is estimated that 95% of people with factor V Leiden never develop a clot.
Factor V Leiden, as a single gene defect, is present in about 5% of European populations, but it rarely occurs in native Asian or African populations. It is present in 20 to 60% of patients with spontaneous venous thrombosis.
A diagnosis of factor V Leiden thrombophilia may be considered in people with a notable personal or family history of VTE, such as having a VTE at an atypically young age, in an unusual location, or having multiple VTEs.
Anticoagulation with parenteral heparin or low molecular weight heparin, followed by oral warfarin, is used for venous thrombosis or as prophylaxis for patients at increased thrombotic risk (e.g., by immobilisation, severe injury, or surgery).
It is not yet known if the newer oral anticoagulants that inhibit either thrombin (dabigatran) or factor Xa (eg, rivaroxaban “XARELTO”, apixaban “ELIQUIS”) can be used in place of warfarin for this disorder.
Prothrombin 20210 gene mutation:
Prothrombin (factor II) is a vitamin K-dependent precursor of thrombin, the end-product of the coagulation cascade. A mutation of the prothrombin 20210 gene increases plasma prothrombin levels (potentially increasing thrombin generation) and increases the risk of venous thromboembolism.
The prevalence of the mutation ranges from < 1% to 6.5%, depending on the population studied.
The diagnosis is made by genetic analysis of the prothrombin 20210 gene using blood samples.
Anticoagulation with heparin or low molecular weight heparin, followed by warfarin, is used for venous thrombosis or for prophylaxis in patients at increased thrombotic risk (e.g., by immobilisation, severe injury, or surgery).
It is not known if the newer oral anticoagulants that inhibit either thrombin (dabigatran) or factor Xa (eg, rivaroxaban, apixaban) can be used in place of other anticoagulants for this disorder.
Deficiency of protein C:
Protein C is a vitamin K–dependent protein, as are coagulation factors VII, IX, and X, prothrombin, and proteins S and Z. Because activated protein C (APC) degrades factors Va and VIIIa, APC is a natural plasma anticoagulant. Decreased protein C due to genetic or acquired causes promotes venous thrombosis.
Heterozygous deficiency of plasma protein C has a prevalence of 0.2 to 0.5%; about 75% of people with this defect experience venous thromboembolism (50% by age 50).

Neonatal purpura fulminans secondary to homozygous Protein C deficiency presenting with widespread purpuric necrosis and limb ischemia
Homozygous or doubly heterozygous deficiency causes neonatal purpura fulminans, ie, severe neonatal disseminated intravascular coagulation (DIC).
Acquired decreases occur in patients with liver disease or DIC and during warfarin therapy.
Diagnosis is based on antigenic and functional plasma assays.
Patients with symptomatic thrombosis require anticoagulation with heparin or low molecular weight heparin, followed by warfarin. Use of the vitamin K antagonist, warfarin, as initial therapy occasionally causes thrombotic skin infarction by lowering vitamin K–dependent protein C levels before a therapeutic decrease has occurred in most vitamin K–dependent coagulation factors.
It is not known whether the newer oral anticoagulants that inhibit either thrombin (dabigatran) or factor Xa (eg, rivaroxaban, apixaban) can be used in place of other anticoagulants for this disorder.
Neonatal purpura fulminans is fatal without replacement of protein C (using normal plasma or purified concentrate) and anticoagulation with heparin or low molecular weight heparin.
Deficiency of protein S:
Protein S, a vitamin K-dependent protein, is a cofactor for activated protein C–mediated cleavage of factors Va and VIIIa.
Heterozygous plasma protein S deficiency predisposes to venous thrombosis. In genetic transmission, prevalence, laboratory testing, treatment, and precautions, heterozygous protein S deficiency is similar to heterozygous protein C deficiency.
Homozygous deficiency of protein S can cause neonatal purpura fulminans that is clinically indistinguishable from that caused by homozygous deficiency of protein C.
Acquired deficiencies of protein C (and, soon thereafter, protein S) occur during disseminated intravascular coagulation (DIC) and warfarin therapy.
Diagnosis is based on antigenic assays of total or free plasma protein S (free protein S is the form unbound to the protein S carrier molecule, C4-binding protein).
The treatment of protein S deficiency associated with venous thrombosis is identical to that of protein C deficiency, with one exception. Because there is no purified protein S concentrate available for transfusion, normal plasma is used to replace protein S during a thrombotic emergency.
It is not known if the newer oral anticoagulants that inhibit either thrombin (dabigatran) or factor Xa (eg, rivaroxaban, apixaban) can be used in place of other anticoagulants for this disorder.
Deficiency of protein Z:
Protein Z, a vitamin K-dependent protein, functions as a cofactor to down-regulate coagulation by forming a complex with the plasma protein, Z-dependent protease inhibitor (ZPI). The complex predominantly inactivates factor Xa on phospholipid surfaces.
The consequence of protein Z or ZPI deficiency, or of autoantibodies to protein Z, in the pathophysiology of thrombosis and fetal loss is not completely clear; however, either defect may make thrombosis more likely if an affected patient also has another congenital coagulation abnormality (eg, factor V Leiden).
Quantification of protein Z, ZPI, and protein Z autoantibodies is done in specialised regional laboratories by plasma electrophoresis, immunoblotting, and enzyme-linked immunosorbent assay.
It is not yet known whether anticoagulant therapy or prophylaxis is indicated in protein Z or ZPI deficiency.
Antithrombin deficiency:
Antithrombin is a protein that inhibits thrombin and factors Xa, IXa, and XIa, thereby inhibiting thrombosis.
Heterozygous deficiency of plasma antithrombin has a prevalence of about 0.2 to 0.4%; about half of people affected develop venous thromboses. Homozygous deficiency is probably lethal to the fetus in utero.
Acquired deficiencies occur in patients with disseminated intravascular coagulation, liver disease, or nephrotic syndrome, or during heparin therapy. Heparin exerts its anticoagulant effect by activating antithrombin.
Laboratory testing is done for patients with an unexplained blood clot and involves quantification of the capacity of patient plasma to inhibit thrombin in the presence of heparin.
Oral warfarin is used for prophylaxis against venous thromboembolism.
It is not yet known if the newer oral anticoagulants that inhibit either thrombin (dabigatran) or factor Xa (eg, rivaroxaban, apixaban) can be used in place of warfarin in this disorder.
Acquired risk factors for hypercoagulability and thrombosis:
The most common acquired risk factors for hypercoagulability and thrombosis are as follows:
Advanced age and atherosclerosis: Atherosclerosis increases the risk of arterial thrombi. Higher risk in patients with preexisting stenosis. When atherosclerotic plaques rupture, they expose or release tissue factor, activate coagulation, initiate local platelet adhesion and aggregation, and cause thrombosis.
Immobilisation: Prolonged immobilisation and advanced age are considered to be important risk factors for VTE. Nevertheless, the need for VTE prophylaxis in long-term bedridden patients is not known. Venous stasis due to surgery, orthopaedic or paralytic immobilisation, heart failure, pregnancy, or obesity is a risk factor for VTE.
Inflammation: Systemic inflammation is a potent prothrombotic stimulus. Inflammatory mechanisms upregulate procoagulant factors, downregulate natural anticoagulants and inhibit fibrinolytic activity. In addition to modulating plasma coagulation mechanisms, inflammatory mediators appear to increase platelet reactivity. In vivo, however, natural anticoagulants not only prevent thrombosis, but they also dampen inflammatory activity.
Infection, if severe (eg, sepsis): Increases risk of venous thrombosis. Increases expression/exposure of tissue factor by monocytes and macrophages.
Pregnancy: Pregnant women are more likely to develop thrombosis than non-pregnant women of the same age. A clot can form at any stage of pregnancy and up to six weeks after the birth. The most common type of blood clot in pregnancy is deep vein thrombosis (DVT). DVT can appear in the deep veins in the back of the leg, or in the calf or pelvis.
Oral contraceptives that contain oestrogen: VTE is more frequent in patients who have a genetic abnormality that predisposes to venous thromboembolism and in women who smoke.
Hormone replacement therapy (HRT): the risk of venous thromboembolism (VTE) is increased by oral HRT compared with baseline population risk. The risk of VTE associated with HRT is greater for oral than transdermal preparations. The risk associated with transdermal HRT given at standard therapeutic doses is no greater than baseline population risk. Consider transdermal rather than oral HRT for menopausal women who are at increased risk of VTE, including those with a BMI over 30 kg/m2. Consider referring menopausal women at high risk of VTE (for example, those with a strong family history of VTE or a hereditary thrombophilia) to a haematologist for assessment before considering HRT.
Smoking appears to be a risk factor for venous thrombosis with the greatest relative effect among young women using oral contraceptives.
Obesity: Obesity appears to be independently associated with both arterial and idiopathic venous thrombotic events. There are several mechanisms through which obesity can mediate its effects. The pro-thrombotic factors associated with obesity have been shown to improve with weight loss indicating that obesity is a modifiable risk factor for thrombosis.
Diabetes: Atherothrombosis is the leading cause of morbidity and mortality in patients with diabetes mellitus. Several mechanisms contribute to the diabetic prothrombotic state, including endothelial dysfunction, coagulative activation and platelet hyper-reactivity. In particular, diabetic platelets are characterised by dysregulation of several signaling pathways leading to enhanced adhesion, activation and aggregation. These alterations result from the interaction among hyperglycemia, insulin resistance, inflammation and oxidative stress.
Given the high prevalence of obesity and diabetes in the United States and the ageing of the population, the incidence of thrombosis is likely to increase.
Cancer (especially adenocarcinoma): Cancer e.g. promyelocytic leukemia; lung, breast, prostate, pancreas, stomach, and colon tumors may activate coagulation by secreting a factor X–activating protease, by expressing/exposing tissue factor on exposed membrane surfaces, or both.
Sickle cell anemia and other hemolytic anemias: Venous thromboembolism (VTE) is common in patients with sickle cell disease (SCD). The aetiology of increased risk of VTE in SCD patients is multifactorial and is related to both traditional factors and SCD-specific factors. Traditional risk factors such as central venous catheters, frequent hospitalisation, orthopaedic surgeries for avascular necrosis, and pregnancy may lead to increased incidence of VTE in the SCD population. In addition, SCD itself appears to be a hypercoagulable state, and many SCD-specific factors such as thrombophilic defects, genotype and splenectomy may modify the risk of VTE. SCD complications such as acute chest syndrome and pulmonary hypertension may also be related to VTE. Anticoagulation experts should be aware of these factors to help inform prophylaxis and treatment decisions.
Hyperhomocysteinemia: may predispose to arterial thrombosis and venous thromboembolism, possibly because of injury to vascular endothelial cells. Some experts believe, however, that there is insufficient evidence definitively to link hyperhomocysteinemia to thrombosis. Plasma homocysteine levels are elevated ≥ 10-fold in homozygous cystathionine beta-synthase deficiency. Milder elevations occur in heterozygous deficiency and in other abnormalities of folate metabolism, including methyltetrahydrofolate dehydrogenase deficiency. The most common causes of hyperhomocysteinemia are acquired deficiencies of Folate, Vitamin B12, or Vitamin B6 (pyridoxine). Folate deficiency is rare in the Western world due to folate fortification of wheat flour. The abnormality is established by measuring plasma homocysteine levels. Plasma homocysteine levels may be normalised by dietary supplementation with folate, vitamin B12, or vitamin B6 alone or in combination; however, it is not been shown that this therapy reduces the risk of arterial or venous thrombosis.
Heparin-induced thrombocytopenia: The pathophysiology involves antibody formation against the heparin-platelet factor 4 complex, with resultant thrombosis. Thrombosis is usually venous, in the form of deep venous thrombosis or pulmonary embolism, but can be arterial as well, in the form of myocardial infarction or stroke.
Antiphospholipid Syndrome:
Antiphospholipid Syndrome (APS) is an important recognised cause of acquired treatable thrombophilia. It is characterised by the core clinical manifestations of thrombosis in both venous and arterial circulation resulting in recurrent thrombotic events, thrombocytopenia, and in women, it can also be associated with recurrent pregnancy losses and a major cause of pregnancy morbidity. Because thrombosis in APS can occur at almost any site, it is a condition that is seen in almost all medical specialities.
APS occurs either as a primary condition or in the setting of an underlying systemic autoimmune disease, particularly systemic lupus erythematosus (SLE).
Clinical manifestations of APS:

Livedo reticularis presenting as a mottled, reticular skin pattern associated with thrombotic disorders and antiphospholipid syndrome
* Superficial and deep vein thrombosis, cerebral venous thrombosis, retinal vein thrombosis.
* Signs and symptoms of intracranial hypertension, pulmonary emboli, pulmonary arterial hypertension, and Budd-Chiari syndrome.
* Livedo reticularis.
* Arterial thrombosis – migraines, cognitive dysfunction, transient ischemic attacks, stroke, myocardial infarction, ischemic leg ulcers, digital gangrene, avascular necrosis of bone, retinal artery occlusion, renal artery stenosis, and, infarcts of spleen, pancreas, and adrenals.
* Premature atherosclerosis – a rare feature of APS.
* Coombs-positive hemolytic anemia and thrombocytopenia.
* Libman-Sacks endocarditis.
* Fetal loss does not appear to be explained by thrombosis, but rather seems to stem from antibody-mediated interference with the growth and differentiation of trophoblasts, leading to a failure of placentation.
* Discontinuation of therapy, major surgery, infection, and trauma may trigger Catastrophic APS.

Gross pathological specimen demonstrating Libman-Sacks endocarditis with sterile vegetations on the cardiac valve
Diagnosis of APS:
One clinical + one laboratory criterion:
Clinical criteria:
* Vascular thrombosis in any tissue or organ.
* Pregnancy morbidity: One or more unexplained deaths of a morphologically normal fetus at or beyond the tenth week of gestation, One or more premature births of a morphologically normal neonate before the thirty-fourth week of gestation because of eclampsia, severe preeclampsia, or placental insufficiency, A 3 or more unexplained consecutive spontaneous abortions before the 10th week of gestation.
Laboratory criteria:
Characteristic laboratory abnormalities in APS include persistently elevated levels of IgG and IgM antibodies directed against membrane anionic phospholipids or their associated plasma proteins or evidence of a circulating anticoagulant.
The confirmed presence of a repeated antiphospholipid (aPL) antibodies – at intermediate or high titres on two or more occasions, 12 weeks apart is a required criterion for diagnosis of APS:
* Antibodies against cardiolipin – aCL.
* Antibodies against beta 2 glycoprotein I – B2GPI.
* Lupus anticoagulant – LA.
The lupus anticoagulant (LA) is suspected if the APTT is prolonged and does not correct immediately upon 1:1 mixing with normal plasma but does return to normal upon the addition of an excessive quantity of phospholipids (done in the clinical pathology laboratory).
Treatment of APS:
After the first thrombotic event, patients should be placed on warfarin for life aiming to achieve an INR ranging from 2.5 to 3.5, alone or in combination with 75 mg of aspirin daily.
Pregnancy morbidity is prevented by a combination of heparin e.g. enoxaparin with aspirin 75 mg daily. Intravenous immunoglobulin 400 mg/kg daily for 5 days may also prevent abortions, while glucocorticoids are ineffective.
Aspirin 75 mg daily protects patients with SLE positive for aPL antibodies from developing thrombotic events.
It is not yet known if the newer oral anticoagulants that inhibit either thrombin (dabigatran) or factor Xa (eg, rivaroxaban, apixaban) can be used in place of heparin or warfarin for this disorder.
Many patients with coexisting SLE are also treated with hydroxychloroquine (HCQ), which may have some benefit for patients at risk for complications of APS.
Warfarin is contraindicated in pregnancy, as it passes through the placental barrier and may cause bleeding in the fetus; warfarin use during pregnancy is commonly associated with spontaneous abortion, stillbirth, neonatal death, and preterm birth.
Possible causes of pain or swelling of the lower limb:
Venous
Deep vein thrombosis
Superficial thrombophlebitis
Post-thrombotic syndrome
Chronic venous insufficiency
Venous obstruction
Other
Cellulitis
Baker’s cyst
Torn gastrocnemius muscle
Fracture
Haematoma
Acute arterial ischaemia
Lymphoedema
Hypoproteinaemia (for example, cirrhosis, nephrotic syndrome)
Idiopathic (unprovoked) venous thrombotic events are defined as the occurrence of venous thrombosis in the absence of any of the risk factors listed above. About 50% of patients presenting with a first idiopathic venous thrombosis have an underlying thrombophilia.
Diagnosis of VTE:
Wells’ clinical probability tool:
Not a definitive test but should be determined in all patients with suspected DVT. Wells’ criteria are the most widely accepted algorithm used in the clinical diagnosis of DVT.
If the Wells’ score is 2 or greater, the condition is likely (absolute risk is approximately 40%). People with a score of <2 are unlikely to have a DVT (probability <15%).
The criteria are as follows:
* Active cancer (any treatment within past 6 months): 1 point
* Calf swelling where affected calf circumference measures >3 cm more than the other calf (measured 10 cm below tibial tuberosity): 1 point
* Prominent superficial veins (non-varicose): 1 point
* Pitting oedema (confined to symptomatic leg): 1 point
* Swelling of entire leg: 1 point
* Localised pain along distribution of deep venous system: 1 point
* Paralysis, paresis, or recent cast immobilisation of lower extremities: 1 point
* Recent bed rest for >3 days or major surgery requiring regional or general anaesthetic within past 12 weeks: 1 point
* Previous history of DVT or PE: 1 point
* Alternative diagnosis at least as probable: subtract 2 points
This test has not been validated in the pregnant population and, therefore, should not be routinely used to risk stratify a pregnant woman with a suspected DVT. A clinical prediction rule, termed the LEFt score, has been developed specifically for the pregnant population; however, this rule has yet to be rigorously validated and should also not be used routinely.
Quantitative D-dimer level:
Indicated if the pre-test probability of DVT is classified as unlikely (Wells’ score <2). If the D-dimer is normal, DVT is excluded in low-probability patients. If elevated, a venous duplex ultrasound is indicated for further investigation.
Venous Duplex Ultrasound (DUS):
Assesses venous flow by the use of Doppler and vein compression. First-line test in all high-probability patients (Wells’ score of 2 or more) or in low-probability patients (Wells’ score <2) with an elevated D-dimer level to assess popliteal, deep femoral, femoral, and common femoral veins. High sensitivity and specificity of over 95%. Ultrasound cannot provide the exact age of a vein clot, but it is better than all current imaging techniques in differentiating acute, subacute, chronic, and age-indeterminant venous thrombi. The initial test of choice for a pregnant woman suspected of having a DVT. The American College of Chest Physicians (ACCP) advocates the use of serial, proximal ultrasonography if a DVT is suspected in pregnant women.
CT abdomen and pelvis with contrast:
More accurate than ultrasound for visceral veins and deep veins of abdomen and pelvis.
Magnetic resonance venography and CT venography:
May be useful adjuncts, and may be helpful in ascertaining the extent of the DVT.
CT pulmonary angiography (CTPA):
Will show filling defects within the pulmonary vasculature with acute pulmonary emboli. When observed in the axial plane this has been described as the polo mint sign. The central filling defect from the thrombus is surrounded by a thin rim of contrast, appearing like the popular sweet, the polo mint.
Thrombophilia Screen:
Consider testing for hereditary thrombophilia in patients who have had unprovoked DVT or PE and who have a first-degree relative who has had DVT or PE if it is planned to stop anticoagulation treatment.
Antiphospholipid Antibodies:
Consider testing for antiphospholipid antibodies in patients who have had unprovoked DVT or PE if it is planned to stop anticoagulation treatment.
Investigations For Cancer:
Offer all patients diagnosed with unprovoked DVT or PE, who are not already known to have cancer, the following investigations for cancer: a physical examination (guided by the patient’s full history), CXR, blood tests (FBC, serum calcium and LFTs) and urinalysis.
Consider further investigations for cancer, with an abdomino-pelvic CT scan (and a mammogram for women), in all patients aged over 40 years with a first unprovoked DVT or PE who do not have signs or symptoms of cancer based on initial investigation.
JAK2 Mutation:
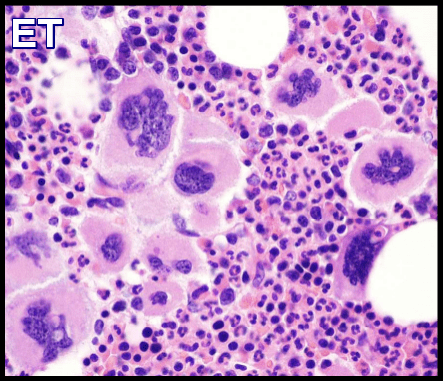
Given that many cases of thrombosis do not have a clear cause, a myeloproliferative neoplasm could be involved. Thromboses are common in patients with polycythemia vera (PV) or essential thrombocythemia (ET). n a few patients, a myeloproliferative disorder (MPD) has been demonstrated to be present, especially in those in whom the thrombosis has occurred in an unusual location, such as in Budd-Chiari syndrome. Investigations to determine the presence of the single point mutation (V617F) of JAK2 are now readily available. This genetic study should be reserved for special cases, such as patients with thrombosis in uncommon sites or patients with cell counts suggesting the presence of a MPD.
Management of VTE:
Refer people who are likely to have DVT for same-day assessment and management (local protocols may vary).
Anticoagulation:
Offer a choice of low molecular weight heparin (LMWH) or fondaparinux to patients with confirmed proximal DVT or PE, taking into account comorbidities and contra-indications, with the following exceptions:
* For patients with severe renal impairment or chronic kidney disease Stage 4 or 5 (estimated glomerular filtration rate <30 ml/min/1.73 m2), offer unfractionated heparin (UFH) with dose adjustments based on the activated partial thromboplastin time (aPTT) or LMWH with dose adjustments based on an anti-Xa assay.
* For patients with an increased risk of bleeding, consider UFH.
* Start the LMWH, fondaparinux or UFH as soon as possible and continue it for at least five days (or for those starting warfarin, until the international normalised ratio (INR) is 2 or above for at least 24 hours, whichever is longer.
* Offer LMWH to patients with active cancer and confirmed proximal DVT or PE and continue the LMWH for six months. At six months, assess the risks and benefits of continuing anticoagulation.
* Offer an oral anticoagulant to patients with confirmed proximal DVT or PE within 24 hours of diagnosis and continue for three months. Traditionally, the oral coagulant has been a vitamin K antagonist, usually warfarin. Recently, however, NICE has approved the novel non-anti-vitamin K antagonist anticoagulants (NOACs) – rivaroxaban, dabigatran, and apixaban – for use in the treatment and secondary prevention of DVT and PE.
* NOACs remain under close scrutiny but many reviews suggest their advantages (most importantly the lack of necessity for monitoring, rapid onset and fewer interactions) outweigh disadvantages (particularly expense and the lack of an immediately acting antidote).
* At three months, assess the risks and benefits of continuing anticoagulant treatment.
Consider extending the anticoagulant beyond three months for patients with unprovoked proximal DVT if their risk of VTE recurrence is high and there is no additional risk of major bleeding.
* Consider catheter-directed thrombolytic therapy for patients with symptomatic iliofemoral DVT who have symptoms of less than 14 days in duration, good functional status, a life expectancy of one year or more and a low risk of bleeding.
* Provide patients who are having anticoagulation treatment with an ‘anticoagulant information booklet’ and an ‘anticoagulant alert card’ and advise them to carry the ‘anticoagulant alert card’ at all times.
Other Management:
* Do not offer below-knee graduated compression stockings unless to manage symptoms.
* Offer temporary inferior vena caval filters to patients with proximal DVT or PE who cannot have anticoagulation treatment; remove the inferior vena caval filter when the patient becomes eligible for anticoagulation treatment.
* Consider inferior vena caval filters for patients with recurrent proximal DVT or PE despite adequate anticoagulation treatment, only after considering alternative treatments such as increasing target INR to 3-4 for long-term high-intensity oral anticoagulant therapy, or switching treatment to LMWH.
* Thrombolytic therapy directed at the vein, increasingly directly by catheter (catheter-directed thrombolysis, or CDT) has had mixed results in studies. It appears to reduce the risk of post-thrombotic syndrome significantly; however, it is not clear whether it reduces risk of PE or recurrence of DVT.
Prognosis:
* Many individuals who have a first episode of DVT or PE will have a recurrent event.
* Without anticoagulation, the risk recurrence of VTE (DVT or PE) is thought to be 50% within three months of a PE. Risk of recurrence within the first year of a VTE following three months of anticoagulation is thought to be 8%.
* Risk of recurrence is reduced by the use of compression stockings.
* The most serious complication of DVT is PE. The risk of PE is higher in proximal clots.
* Thrombosis of the iliofemoral veins carries a worse prognosis with increased incidence of late clinical complications such as post-thrombotic syndrome.
Post-thrombotic syndrome:
Post-thrombotic syndrome is a chronic venous hypertension, which may result in pain, swelling, hyperpigmentation, dermatitis, ulcers, gangrene and lipodermatosclerosis.
It may develop after a DVT, due to damage to the deep veins and their valves.
It affects 20-40% of patients after DVT of the lower limb and can have a significant impact on quality of life.
Risks associated with the syndrome include older age, obesity, a history of previous ipsilateral DVT, iliofemoral location of the current thrombosis, failure to recover promptly from the acute symptoms and insufficient quality of oral anticoagulant therapy.
There is a low risk of post-thrombotic syndrome in patients with asymptomatic DVT.
Prevention of VTE:
VTEs often are preventable, with strategies that stop the development of clots in people “at-risk”. Healthcare professionals discern risk by gathering information about a patient’s age, weight, medical history, medications and lifestyle factors.
The National Institute for Health and Care Excellence (NICE) has produced guidelines to assist in reducing the risk.
NICE states that approximately 30% of surgical patients develop deep vein thrombosis (DVT). The condition is frequently asymptomatic but can lead to sudden death due to pulmonary embolism (PE). The risk of fatal embolism after high-risk surgery is 1-5%.
The following surgical procedures are high-risk:
Orthopaedic surgery (for example, total surgery for hip fracture).
Major general surgery.
Major gynaecological surgery (but not caesarean).
Urological surgery (including major or open urological procedures).
Neurosurgery.
Cardiothoracic surgery.
Major peripheral vascular surgery.
Those at risk may take anti-clotting, or blood-thinning, medications or use mechanical devices such as compression stockings or compression devices. Getting out of bed quickly after surgery is also advised if possible.
Avoid dehydration unless there is a specific clinical reason.
Encourage early mobilisation.
Aspirin or antiplatelet agents should not be considered adequate prophylaxis.
Consider temporary inferior vena cava filters for patients at a very high risk of VTE (eg, active malignancy or previous VTE event) if there are contra-indications to pharmacological and mechanical prophylaxis. These are devices which can be inserted into the inferior vena cava to prevent the development of a pulmonary embolus.
There are currently no randomised controlled trials or controlled clinical trials that have assessed the benefit(s) of testing for thrombophilia on the risk of recurrent VTE.
Summary:
Thrombotic disorders refer to conditions characterized by abnormal blood clot formation within arteries or veins, leading to partial or complete vascular occlusion. These disorders include deep vein thrombosis (DVT), pulmonary embolism (PE), ischemic stroke due to cerebral arterial thrombosis, coronary thrombosis causing myocardial infarction, mesenteric vein thrombosis, renal vein thrombosis, and microvascular thrombosis such as neonatal purpura fulminans due to homozygous Protein C deficiency. Both venous and arterial thrombotic events may arise from inherited thrombophilia, antiphospholipid syndrome, malignancy, or acquired hypercoagulable states.
Thrombosis occurs when the normal balance of haemostasis is disrupted, typically involving elements of Virchow’s triad: endothelial injury, hypercoagulability, and blood flow stasis. Venous thrombosis is primarily fibrin-rich and associated with immobility, surgery, malignancy, inherited thrombophilia, and antiphospholipid syndrome. In contrast, arterial thrombosis is platelet-driven and commonly related to atherosclerosis and plaque rupture.
Clinical manifestations vary depending on the vascular territory involved. DVT presents with unilateral leg swelling and pain. PE may show the classic “polo mint sign” on CTPA. Mesenteric vein thrombosis presents with abdominal pain and ischemia. Renal vein thrombosis causes flank pain and renal dysfunction. Coronary thrombosis leads to acute coronary syndromes. Cutaneous markers such as livedo reticularis and systemic findings such as Libman–Sacks endocarditis may indicate underlying autoimmune or thrombotic pathology.
Early diagnosis using duplex ultrasonography, CT angiography, or MRI, combined with risk stratification for thrombophilia or malignancy, is essential. Management includes anticoagulation, treatment of underlying causes, and long-term prevention of recurrence.
Questions and Answers:
What are thrombotic disorders?
Thrombotic disorders are medical conditions in which abnormal blood clots form inside arteries or veins, leading to partial or complete vascular occlusion and potential organ damage.
What is the difference between venous and arterial thrombosis?
Venous thrombosis, such as deep vein thrombosis (DVT) or mesenteric vein thrombosis, is typically fibrin-rich and associated with blood stasis and hypercoagulability. Arterial thrombosis, such as coronary or cerebral thrombosis, is platelet-driven and commonly linked to atherosclerosis and endothelial injury.
What are the symptoms of deep vein thrombosis (DVT)?
DVT typically presents with unilateral leg swelling, calf pain, warmth, erythema, and tenderness. If untreated, it may progress to pulmonary embolism.
What is pulmonary embolism (PE)?
Pulmonary embolism is a potentially life-threatening condition in which a blood clot, usually originating from a deep vein thrombosis, travels to and obstructs the pulmonary arteries, causing shortness of breath, chest pain, tachycardia, and hypoxia.
What is the polo mint sign in pulmonary embolism?
The polo mint sign on CT pulmonary angiography represents a central intraluminal thrombus surrounded by contrast material within a pulmonary artery, confirming the presence of pulmonary embolism.
Can thrombotic disorders cause stroke?
Yes. Thrombotic disorders can cause ischemic stroke when a blood clot forms within a cerebral artery or embolizes to the brain, leading to interruption of cerebral blood flow and infarction.
What is the difference between thrombotic stroke and embolic stroke?
A thrombotic stroke occurs when a clot forms directly within a cerebral artery, often due to atherosclerosis. An embolic stroke occurs when a clot forms elsewhere, such as in the heart, and travels to the brain. Both are forms of arterial thrombosis.
How are thrombotic strokes treated?
Acute management may include intravenous thrombolysis or mechanical thrombectomy when appropriate. Long-term secondary prevention depends on the underlying cause and may involve antiplatelet therapy or anticoagulation.
How are thrombotic disorders treated?
Treatment typically involves anticoagulation therapy such as direct oral anticoagulants (DOACs), low-molecular-weight heparin, or warfarin. Management also includes addressing underlying risk factors and determining the duration of therapy based on recurrence risk.
When should thrombophilia testing be considered?
Thrombophilia testing should be considered in patients under 40 years with unprovoked thrombosis, recurrent thrombotic events, thrombosis at unusual sites, or a strong family history of thrombotic disorders.
When should thrombophilia testing be considered in stroke patients?
Testing may be considered in patients under 50 years with unexplained ischemic stroke, recurrent arterial events, or clinical features suggestive of antiphospholipid syndrome or inherited hypercoagulability.
When should cancer be suspected in a patient with thrombosis?
Occult malignancy should be considered in patients over 50 years presenting with unprovoked venous thromboembolism, particularly in the absence of identifiable risk factors or in cases of recurrent or unusual-site thrombosis.
What causes mesenteric vein thrombosis?
Mesenteric vein thrombosis may result from inherited thrombophilia, antiphospholipid syndrome, malignancy, inflammatory bowel disease, liver disease, or other hypercoagulable states and typically presents with abdominal pain.
What is neonatal purpura fulminans?
Neonatal purpura fulminans is a severe thrombotic condition caused by homozygous Protein C deficiency, leading to widespread microvascular thrombosis, skin necrosis, and disseminated intravascular coagulation shortly after birth.
What is livedo reticularis a sign of?
Livedo reticularis is a mottled, net-like skin discoloration that may indicate underlying vascular obstruction and is commonly associated with antiphospholipid syndrome or systemic thrombotic disease.
References:
Furie B, Furie BC. Mechanisms of thrombus formation. N Engl J Med. 2008;359(9):938–949.
Goldhaber SZ, Bounameaux H. Pulmonary embolism and deep vein thrombosis. Lancet. 2012;379(9828):1835–1846.
Prandoni P, Kahn SR. Post-thrombotic syndrome: prevalence, prognostication, and need for progress. Br J Haematol. 2009;145(3):286–295.
Mekaj YH, Mekaj AY, Duci SB, et al. New oral anticoagulants: advantages and disadvantages compared with vitamin K antagonists in prevention and treatment of thromboembolic events. Ther Clin Risk Manag. 2015;11:967–977. doi:10.2147/TCRM.S84210.
Watson L, Broderick C, Armon MP. Thrombolysis for acute deep vein thrombosis. Cochrane Database Syst Rev. 2014;1:CD002783. doi:10.1002/14651858.CD002783.pub3.
NICE. Venous thromboembolic diseases: diagnosis, management and thrombophilia testing (CG144). London: National Institute for Health and Care Excellence; 2012 (updated 2015).
NICE. Venous thromboembolism in adults admitted to hospital: reducing the risk (CG92). London: NICE; 2010.
NICE. Apixaban, rivaroxaban, and dabigatran for treatment and secondary prevention of DVT and PE (TA261, TA327, TA341). London: NICE; 2012–2015.
Negrini S, Pappalardo F, Murdaca G, et al. The antiphospholipid syndrome: from pathophysiology to treatment. Clin Exp Med. 2016.
Nayfe R, Uthman I, Aoun J, et al. Seronegative antiphospholipid syndrome. Rheumatology (Oxford). 2013;52(8):1358–1367.
Darvall KAL, Sam RC, Silverman SH, et al. Obesity and thrombosis. Eur J Vasc Endovasc Surg. 2007;33(2):223–233.
Breccia M, Morano SG, D’Andrea M, et al. Budd–Chiari syndrome as first manifestation of polycythemia vera in young women with inherited thrombophilia. Eur J Haematol. 2005;75:396–400.
Useche JN, de Castro AM, Galvis GE, et al. Ultrasonography in evaluation of deep vein thrombosis. Radiographics. 2008;28(6):1785–1797.
Michiels JJ, Oortwijn WJ, Naaborg R. Rapid ELISA D-dimer test and compression ultrasonography for DVT diagnosis. Clin Appl Thromb Hemost. 1999;5(3):171–180.
Moake JL. Overview of thrombotic disorders. Merck Manual Professional Edition.
Schick P. Hereditary and acquired hypercoagulability. Medscape Reference.
Keywords:
thrombotic disorders, thrombosis, blood clot disorder, venous thrombosis, arterial thrombosis, deep vein thrombosis DVT, pulmonary embolism PE, ischemic stroke thrombosis, cerebral arterial thrombosis, coronary thrombosis, myocardial infarction clot, mesenteric vein thrombosis, renal vein thrombosis, Budd Chiari syndrome, hypercoagulable state, thrombophilia, inherited thrombophilia, acquired thrombophilia, antiphospholipid syndrome APS, seronegative antiphospholipid syndrome, protein C deficiency, homozygous protein C deficiency, protein S deficiency, antithrombin deficiency, factor V Leiden mutation, prothrombin gene mutation G20210A, thrombophilia workup, thrombophilia screen, thrombophilia testing indications, thrombophilia in pregnancy, recurrent miscarriage thrombophilia, thrombophilia pregnancy loss, thrombophilia and stroke, thrombophilia and cancer, occult malignancy and thrombosis, venous thromboembolism VTE, DVT symptoms, pulmonary embolism symptoms, polo mint sign CTPA, D dimer test, compression ultrasonography DVT, anticoagulation therapy, DOACs, rivaroxaban, apixaban, dabigatran, warfarin therapy, heparin treatment, thrombolysis for DVT, mechanical thrombectomy stroke, post thrombotic syndrome, livedo reticularis, Libman Sacks endocarditis, neonatal purpura fulminans, microvascular thrombosis, disseminated intravascular coagulation DIC, Virchow triad, thrombosis risk factors, obesity and thrombosis, cancer associated thrombosis, thrombosis management guidelines


Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now





Hi
My name is Lisa Johnson
I am at risk and need to find thrombotic disease hematologist. I am in south Florida
Hi Lisa,
Thank you for your message.
Unfortunately, I am based in London but you can email your query to in**@*************st.com
Best wishes,