Lupus Erythematosus (LE) Cells
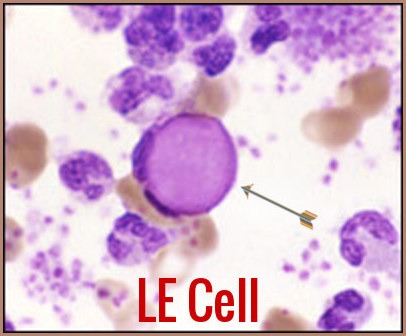
LE cell in lupus erythematosus demonstrating the engulfed homogeneous LE body characteristic of SLE.
Lupus Erythematosus (LE) cells are characteristic neutrophils that have phagocytosed the denatured nuclear material of damaged lymphocytes, typically coated with autoantibodies against nucleoproteins. First identified by Dr. Robert H. Heitzman in 1948, LE cells once served as a key diagnostic marker for systemic lupus erythematosus (SLE), reflecting the autoimmune pathophysiology of the disease. Although largely replaced today by more sensitive serologic tests such as ANA and anti-dsDNA, LE cells remain an important historical and morphological indicator in the understanding and diagnosis of lupus and related autoimmune conditions.
The Lupus Erythematosus (LE) cell was so termed because of its exclusive presence in the bone marrow of 25 patients with confirmed or suspected SLE at the Mayo Clinic. The first three cases were children, the first a 9‐yr‐old with, very unusually, hypergammaglobulinaemia, plasmacytosis and Bence‐Jones proteinuria; the second, also 9‐yr‐old, with unexplained anaemia and purpura, and the third a boy with cryoglobulinaemia and purpura.
A more conclusive link with SLE came after the LE cell phenomenon was observed in the marrow of a patient with classical SLE in 1948 by Hargraves et al.
Lupus Erythematosus (LE) Cells are not usually found in peripheral blood, although Sundberg and Lick, also at the Mayo Clinic, observed in 1949 that the LE cell phenomenon could form in the buffy coat of peripheral blood after a period of incubation at room temperature while rotating with glass beads.
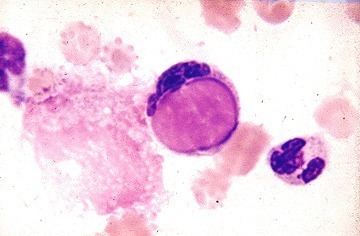
A peripheral blood smear from a patient with systemic lupus erythematosus demonstrating a classic LE cell, where a neutrophil has engulfed denatured nuclear material forming a homogeneous LE body. Note the adjacent normal neutrophil and surrounding nuclear debris. Courtesy of the American College of Rheumatology.
Lupus Erythematosus (LE) Cells have since been found in synovial fluid, cerebrospinal fluid and pericardial and pleural effusions from patients with SLE.
The LE cell reaction is positive in 50%-75% of individuals with acute disseminated systemic Lupus Erythematosus (SLE). Positive reactions are also seen in rheumatoid arthritis, chronic hepatitis, scleroderma, dermatomyositis, polyarteritis nodosa, acquired hemolytic anemia, and Hodgkin’s disease. It may also be positive in persons taking phenylbutazone and hydralazine.
Lupus erythematosus (LE) cell testing was once performed to diagnose systemic lupus erythematous but has been replaced for this purpose by antinuclear antibody testing.
Negative findings on Lupus Erythematosus (LE) cell testing exclude a diagnosis of systemic lupus erythematosus (SLE).
The presence of LE cells indicates lupus.
A smear is considered positive when ten or more characteristic LE cells are seen during a 15-minute search associated with the presence of extracellular, amorphous, nuclear masses.

Blood film demonstrating a classic LE cell in lupus erythematosus, where a neutrophil engulfs a dense homogeneous LE body (red arrow), characteristic of SLE.
The discovery of the LE cell phenomenon remains a fundamental observation in the pathogenesis of SLE. Along with the VDRL test, the LE cell preparation remains in the American College of Rheumatology’s criteria for the classification of SLE.
It’s important to note that while the presence of LE cells is strongly associated with SLE, their absence does not rule out the disease. However, the test has been largely replaced by the antinuclear factor test (ANF) and DNA binding assays.
An interesting article published in J Cytol. 2012 Jan-Mar; 29(1): 77–79, reported an unusual case of SLE in a 16-year-old female who presented with acute shortness of breath, fever and cough. Her chest radiograph showed bilateral pleural effusion. This effusion was tapped and sent to the cytopathology laboratory. The cytological examination of the pleural fluid revealed numerous LE cells and led to the diagnosis of SLE.
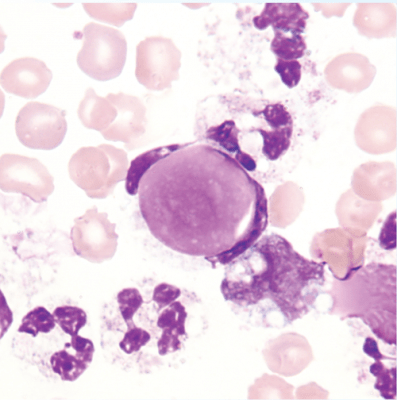
Blood film from a patient with lupus erythematosus showing a well-formed LE cell containing a dense, homogeneous LE body produced by immune-mediated nuclear material ingestion.
Clinical Significance:
The presence of LE cells in the peripheral blood is a diagnostic feature of SLE. However, the sensitivity and specificity of this test are relatively low, and LE cells can also be found in other conditions, such as infections, malignancies, and drug-induced lupus. Therefore, the diagnosis of SLE should be based on a combination of clinical features, laboratory tests, and imaging studies.
In addition to their diagnostic significance, LE cells have been implicated in the pathogenesis of SLE. The phagocytosis of antibody-coated nuclear material by neutrophils and other phagocytic cells can lead to the release of pro-inflammatory cytokines and other mediators that can contribute to the development of tissue damage and organ dysfunction in SLE.
Summary:
Lupus erythematosus (LE) cells represent a classic hematologic hallmark of systemic lupus erythematosus (SLE), formed when neutrophils engulf antibody-coated, denatured nuclear material to create the distinctive homogeneous LE body. Although modern diagnostics rely primarily on ANA, anti-dsDNA, ENA panels, and other immunologic markers, LE cells remain an important historical and morphological indicator of lupus activity. Their presence in blood or bone marrow reflects underlying immune complex formation and nuclear antigen targeting—a fundamental pathogenic mechanism in SLE. This post reviews the origin, formation, clinical relevance, diagnostic role, morphology, and limitations of LE cell testing, supported by high-quality microscopic images that illustrate classic LE cell features for clinicians, trainees, and laboratory professionals.
Questions and Answers:
What is an LE cell in systemic lupus erythematosus?
An LE cell is a neutrophil that has engulfed antibody-coated, denatured nuclear material from a damaged lymphocyte, forming a smooth, homogeneous structure known as an LE body—historically used as a diagnostic marker for SLE.
How do LE cells form in lupus erythematosus?
LE cells form when antinuclear antibodies bind nuclear debris, creating immune complexes that are subsequently phagocytosed by neutrophils, resulting in the characteristic spherical LE body.
Are LE cells still used to diagnose lupus today?
LE cell testing is largely obsolete and has been replaced by more sensitive and specific assays such as ANA, anti-dsDNA, and ENA panels, though LE cells remain useful for historical and educational context.
What does an LE cell look like under the microscope?
Microscopically, an LE cell appears as a neutrophil containing a large, smooth, round, purple LE body that displaces the neutrophil’s original nucleus to the cell periphery.
What is the clinical significance of LE cells in SLE?
The presence of LE cells reflects underlying immune dysregulation and nuclear antigen targeting in lupus, illustrating a key pathogenic process, although it is no longer required for diagnosis.
Why was the LE cell test replaced by ANA testing?
ANA testing offers far greater sensitivity, broader antigen detection, automation, and standardisation, making it superior to the labor-intensive and less sensitive LE cell preparation method.
Can LE cells appear in diseases other than SLE?
Yes, LE cells may rarely be seen in other autoimmune conditions such as rheumatoid arthritis, drug-induced lupus, and certain connective tissue diseases, though far less commonly than in SLE.
What is the difference between an LE cell and a tart cell?
A tart cell is a phagocyte that has ingested intact lymphocyte nuclei with visible chromatin, whereas an LE cell contains fully denatured, homogeneous nuclear material bound by antinuclear antibodies.
Do LE cells correlate with lupus disease activity?
LE cells are not reliable markers of disease activity and are not used for monitoring; modern markers such as complement levels, anti-dsDNA titres, ESR/CRP, and clinical assessment provide more accurate evaluation.
Are LE cells found in blood or bone marrow?
LE cells can be detected in peripheral blood smears or bone marrow preparations, depending on disease severity and the technique used, though both are uncommon in routine practice today.
References:
Hepburn AL. The LE cell. Rheumatology. 2001;40(7):826–827. doi:10.1093/rheumatology/40.7.826
Hargraves MM. Discovery of the LE cell and its morphology. Proc Staff Meet Mayo Clin. 1969;44:579–589.
Hargraves MM, Richmond H, Morton R. Presentation of two bone marrow elements: the “tart” cell and the “LE” cell. Mayo Clin Proc. 1948;23:25–28.
Sundberg RD, Lick NB. LE cells in the blood in acute disseminated lupus erythematosus. J Invest Dermatol. 1949;12:83–84.
Lachmann PJ. A two-stage indirect LE cell test. Immunology. 1961;4:142–152.
Ogryzlo MA. The LE (lupus erythematosus) cell reaction. Can Med Assoc J. 1956;75(12):980–993.
Hepburn AL. The LE cell. Rheumatology. 2001;40(7):826–827.
Tan EM, Cohen AS, Fries JF, et al. The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum. 1982;25:1271–1277.
Lahita RG. Systemic Lupus Erythematosus. Philadelphia: Churchill Livingstone; 1992.
Koffler D, Agnello V, Winchester R. The occurrence of “LE” cells in systemic lupus erythematosus. J Clin Invest. 1971;50:1702–1709.
Pisetsky DS. Immune complexes in rheumatic disease: a review. Clin Immunol Immunopathol. 1989;53:439–449.
Heitzman R. The LE cell. JAMA. 1948;138(10):728–733.
UpToDate. Circulating “LE cell” in systemic lupus erythematosus. Available at: https://www.uptodate.com/contents/image?imageKey=RHEUM%2F62681
Keywords:
lupus erythematosus cells, LE cells, lupus erythematosus cell, LE cell morphology, LE cell phenomenon, LE body hematoxylin body, Hargraves cell lupus, lupus erythematosus cell test, LE cell test principle, lupus erythematosus cell preparation, detecting LE cells blood smear, LE cells diagnosis SLE, systemic lupus erythematosus SLE, SLE blood smear findings, lupus diagnostic markers, what are LE cells, LE cell definition, lupus erythematosus cell found in, lupus autoimmune disease test, lupus blood test interpretation, ANA vs LE cell test, SLE microscopic features, immune complex disease lupus, nuclear material ingestion neutrophil, lupus hematology findings, lupus cytology images, LE body formation, tart cell vs LE cell, lupus erythematosus cell detection, circulating LE cell, lupus cell pathology, LE cell identification, classic LE cell image, LE cell in bone marrow, lupus nuclear antigen reaction, phagocytosed nuclear debris lupus, LE cell formation mechanism, lupus hematology smear, LE cell diagnosis accuracy, lupus screening tests, SLE clinical pathology, autoimmune nuclear antibody complex, lupus morphology under microscope, LE cell historical significance, Hargraves LE cell discovery


Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now

That is really interesting, You’re an overly professional blogger.
I have joined your feed and look ahead to
in search of more of your great post. Also, I’ve shared your site in my social networks