Hemolytic Disease Of The Newborn (HDN)
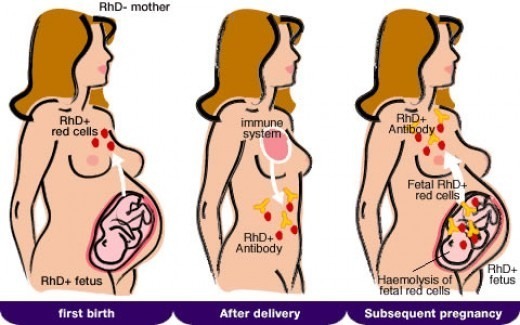
Mechanism of Hemolytic Disease of the Newborn: maternal sensitization to Rh-positive fetal cells and antibody-mediated hemolysis in later pregnancies.
Hemolytic disease of the newborn (HDN) is an alloimmune condition in which maternal IgG antibodies cross the placenta and destroy fetal red blood cells, leading to fetal anemia, hydrops fetalis, jaundice and, historically, significant neonatal mortality. Although the condition was first documented as early as 1609, its true mechanism remained unknown for centuries until the 1950s, when researchers clarified that HDN results from blood group incompatibility between mother and fetus.
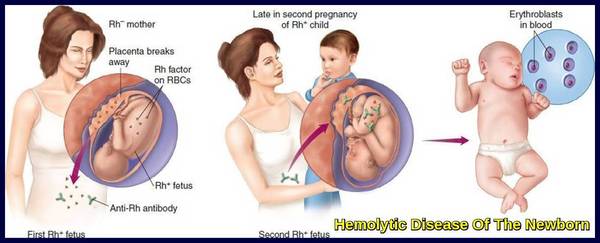
Rh alloimmunization leading to Hemolytic Disease of the Newborn, showing maternal sensitization during a first pregnancy and fetal hemolysis in a later Rh-positive pregnancy.

Hydrops fetalis as a severe manifestation of Hemolytic Disease of the Newborn, with fluid accumulation in multiple fetal compartments.
In subsequent pregnancies with an antigen-positive fetus, maternal IgG antibodies form and cross the placenta, causing hemolysis in the fetus. Most immune-mediated HDN cases are due to antibodies against the Rhesus D antigen. Approximately 15% of births occur to RhD-negative mothers with an RhD-positive father, and around 75% of these infants will be RhD-positive, placing them at risk for alloimmunization and HDN.
The introduction of routine antenatal screening and prophylactic anti-D immunoglobulin in the 1960s and 1970s dramatically reduced the incidence of severe HDN, stillbirth and neonatal death. Today, identifying antigen-negative mothers carrying antigen-positive fetuses, quantifying fetomaternal hemorrhage (e.g., via the Kleihauer test), and providing timely prophylaxis or treatment remain central to preventing morbidity.

Kleihauer–Betke test diagram demonstrating fetomaternal hemorrhage detection and its role in preventing Hemolytic Disease of the Newborn (Source: Osmosis.org).
In subsequent pregnancies with an antigen-positive fetus, IgG antibodies are formed which cross the placenta and cause hemolysis in the fetus. Most cases of immune HDN are due to antibodies to rhesus D antigen. Nearly 15% of births are to rhesus D-negative mothers with a D-positive father and 75% of these children will be D-positive.
Clinical features:

Peripheral blood smear demonstrating erythroblasts and hemolysis in a neonate with Hemolytic Disease of the Newborn.
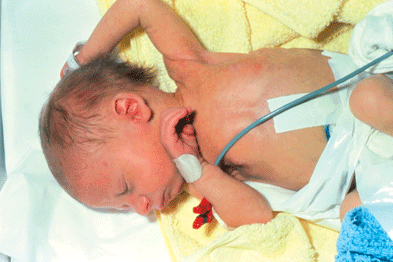
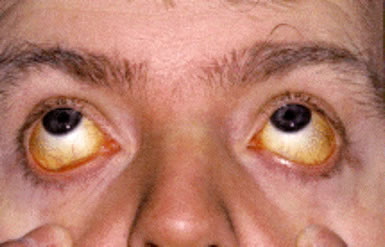
Severe neonatal jaundice in Hemolytic Disease of the Newborn requiring monitoring and supportive care.
- There is anemia in the affected fetus or child associated with nucleated red blood cells (NRBCs) in the neonate’s blood.
- At birth, the child is not severely jaundiced because of the placental clearance system, but jaundice may worsen rapidly and produce kernicterus if not treated promptly.
- In its severest form, there is cardiac failure, hepatosplenomegaly, and intrauterine death (hydrops fetalis).
Diagnosis:
- The blood group of the mother is routinely assessed, and the father is also tested if the mother is D-negative. A previous history of pregnancies, previously affected infants, abortions and blood transfusions (possible sensitization) is essential.
- During the pregnancy Rh positive antibodies can be measured in the maternal serum, and bilirubin can be measured in the amniotic fluid to assess the severity of the hemolysis.
- At birth, the degree of anemia is the best guide to the severity. The blood film reveals increased nucleated RBCs, reticulocytosis, polychromasia, anisocytosis, spherocytes, and cell fragmentation. The reticulocyte count can be as high as 40% in patients without intrauterine intervention.
- Positive maternal indirect Coombs test.
- Positive neonatal direct Coombs test.
- Ultrasound – to detect organ enlargement or fluid buildup in the fetus.
Treatment:
- As a rule, serial maternal antibody titers are monitored until a critical titer of 1:32, which indicates that a high risk of fetal hydrops has been reached. At this point, the fetus requires very intense monitoring for signs of anemia and fetal hydrops.
- In severe cases, intrauterine transfusion must be given. Transfused cells must be compatible with the mother’s serum.
- Exchange transfusion may be required soon after birth to prevent kernicterus. Fresh blood should be used.
- Phototherapy may augment bilirubin breakdown and avoid the necessity of exchange transfusion in mild cases.
Summary:
Hemolytic Disease of the Newborn (HDN) is an alloimmune condition in which maternal IgG antibodies target fetal red blood cells due to blood group incompatibility, most commonly RhD. Sensitization typically occurs when an Rh-negative mother is exposed to Rh-positive fetal cells during pregnancy or delivery, leading to anti-D antibody formation. In subsequent pregnancies with an Rh-positive fetus, these antibodies cross the placenta and cause hemolysis, resulting in fetal anemia, hydrops fetalis, jaundice, and potentially kernicterus if untreated. Diagnosis relies on maternal antibody screening, fetal monitoring, and tests such as the Kleihauer–Betke to quantify fetomaternal hemorrhage. Management includes anti-D immunoglobulin prophylaxis, intensive neonatal monitoring, phototherapy, exchange transfusion, and treatment of severe anemia. Routine antenatal screening and timely prophylaxis have dramatically reduced the incidence and severity of HDN worldwide.
Questions and Answers:
What is Hemolytic Disease of the Newborn?
Hemolytic Disease of the Newborn is an alloimmune condition in which maternal IgG antibodies cross the placenta and destroy fetal red blood cells due to blood group incompatibility, most commonly RhD, leading to fetal anemia, jaundice, and potentially hydrops fetalis.
What causes Hemolytic Disease of the Newborn?
Hemolytic Disease of the Newborn is caused by maternal sensitization to fetal red cell antigens—most often RhD—during pregnancy, delivery, trauma, or invasive procedures, resulting in anti-D antibodies that attack fetal RBCs in subsequent pregnancies.
How does Rh sensitization lead to Hemolytic Disease of the Newborn?
When an Rh-negative mother is exposed to Rh-positive fetal red blood cells, she forms anti-D IgG antibodies. In a later pregnancy with an Rh-positive fetus, these antibodies cross the placenta and cause hemolysis, leading to Hemolytic Disease of the Newborn.
What are the symptoms of Hemolytic Disease of the Newborn?
Key symptoms include jaundice, anemia, pallor, hepatosplenomegaly, elevated bilirubin, and in severe cases hydrops fetalis with ascites, pleural effusion, pericardial effusion, and generalized skin edema.
What is hydrops fetalis in Hemolytic Disease of the Newborn?
Hydrops fetalis is a severe complication of Hemolytic Disease of the Newborn characterized by fluid accumulation in two or more fetal compartments, such as ascites, pleural effusion, pericardial effusion, scalp edema, and skin edema due to profound fetal anemia.
How is Hemolytic Disease of the Newborn diagnosed?
Diagnosis includes maternal antibody screening, Doppler MCA flow for fetal anemia, newborn bilirubin measurement, direct antiglobulin test (DAT), blood smear showing erythroblasts, and tests such as the Kleihauer–Betke to quantify fetomaternal hemorrhage.
What is the Kleihauer–Betke test in Hemolytic Disease of the Newborn?
The Kleihauer–Betke test identifies fetal red blood cells in maternal circulation using acid elution, allowing quantification of fetomaternal hemorrhage and calculation of the appropriate dose of RhoGAM to prevent Hemolytic Disease of the Newborn.
How is Hemolytic Disease of the Newborn treated?
Treatment includes intensive neonatal monitoring, phototherapy for hyperbilirubinemia, intravenous immunoglobulin, and exchange transfusion for severe anemia or high bilirubin, along with fetal intrauterine transfusions when indicated.
How can Hemolytic Disease of the Newborn be prevented?
Prevention relies on administering anti-D immunoglobulin to Rh-negative mothers, routine antenatal screening, assessment of fetomaternal hemorrhage, and timely prophylaxis during pregnancy, after delivery, or after sensitizing events.
Is Hemolytic Disease of the Newborn still common today?
Thanks to routine RhD screening and anti-D prophylaxis, the incidence of Hemolytic Disease of the Newborn has dramatically declined, although cases related to non-D antigens or inadequate prophylaxis still occur.
References:
Bowman JM. Hemolytic disease (erythroblastosis fetalis). In: Creasy RK, Resnik R, eds. Maternal-Fetal Medicine. 4th ed. Philadelphia: WB Saunders; 1999:736–767.
Fasano RM. Hemolytic disease of the fetus and newborn in the molecular era. Semin Fetal Neonatal Med. 2015 Nov 14.
Hernández A, LaFayette K. Kleihauer–Betke Test. Osmosis. Available at: https://www.osmosis.org/answers/Kleihauer-Betke-test. Accessed 6 December 2025.
American College of Obstetricians and Gynecologists’ Committee on Practice Bulletins – Obstetrics; Silver RM. Practice Bulletin No. 181 Summary: Prevention of RhD alloimmunization. Obstet Gynecol. 2017;130(2):481–483. doi:10.1097/AOG.0000000000002226
Luchtman-Jones L, Schwartz AL, Wilson DB. The blood and hematopoietic system. In: Fanaroff AA, Martin RJ, eds. Neonatal-Perinatal Medicine: Diseases of the Fetus and Infant. 8th ed. St. Louis, MO: Mosby; 2006. Vol 2:1287–1356.
Urbaniak SJ, Greiss MA. RhD haemolytic disease of the fetus and the newborn. Blood Rev. 2000;14:44–61.
NCBI Bookshelf. Hemolytic disease of the newborn. Blood Groups and Red Cell Antigens. Available at: https://www.ncbi.nlm.nih.gov/books/NBK2266/
Animated Mnemonics (Picmonic). Hemolytic Disease of the Newborn. Available at: https://www.youtube.com/watch?v=DmBNmFn0MOU
Keywords:
hemolytic disease of the newborn, hdn, erythroblastosis fetalis, rh incompatibility newborn, rhd alloimmunization, abo hemolytic disease newborn, anti-kell hdn, anti-RhE hdn, hdn diagnosis, hdn symptoms, hdn treatment, hydrops fetalis hdn, neonatal jaundice hemolysis, rh sensitization pregnancy, kleihauer betke test hdn, fetomaternal hemorrhage hdn, rhogam prophylaxis, intrauterine transfusion hdn, phototherapy hdn, exchange transfusion hdn, neonatal anemia hemolysis, fetal anemia doppler mca, direct antiglobulin test hdn, neonatal bilirubin hdn, hemolytic disease newborn management, hemolytic disease newborn complications, hdn prevention anti-d, sensitizing events pregnancy rh, maternal alloimmunization hdn, red cell antibodies pregnancy, neonatal hemolytic disease rh


Request Online Consultation With Dr M Abdou
Fee: US$100
Secure payment via PayPal (credit and debit cards accepted)
Pay Now


That was a great post. You did cover many aspects very precisely. I am glad that I came across the post.
thank you very much for good i will like joined your reach for your feature resect